The Core Question: Why Do We Need Robots in the Operating Room?
Imagine walking into an operating room and seeing a towering, multi-armed machine hovering over a surgical table. It looks like a scene from a science fiction movie. However, robotic surgery is now a common reality in hospitals around the world.
But why did scientists decide to put machines into the operating room in the first place? Human surgeons have highly trained, capable hands. The answer lies in the limitations of the human body. Human hands have a natural tremor, human eyes cannot magnify tiny blood vessels on their own, and traditional surgical tools are straight and rigid, making it difficult to operate in tight spaces.

Robotic surgery was developed to solve these problems. It is important to understand early on that these machines are not autonomous. A surgical robot cannot make decisions or perform operations on its own. Instead, it is a highly advanced tool completely controlled by a human surgeon.
This article explores how robotic surgery evolved from military experiments to everyday medical care, what the research says about its effectiveness, and where this technology is heading next.
The Origins: Space, War, and the “Golden Minute”
The history of robotic surgery does not begin in a hospital. It begins with the military and the space program.
In the 1980s, the National Aeronautics and Space Administration (NASA) and the United States Department of Defense faced a unique problem. How do you treat a critically injured astronaut in space or a wounded soldier on a remote battlefield? The proposed solution was telepresence (tell-uh-PREZ-uhns), which is the use of technology to make a person feel as if they are present in a different location.
According to a historical review in the Journal of the Society of Laparoendoscopic Surgeons, the military wanted to change the concept of the “Golden Hour” in trauma care to the “Golden Minute.” Instead of transporting a wounded soldier to a distant hospital, they wanted to bring the operating room to the soldier. They envisioned an armored vehicle equipped with a robotic surgical unit. A skilled surgeon sitting in a safe location miles away could control the robot’s arms to stop bleeding and stabilize the patient immediately.

While this exact military vision was never fully deployed in combat, the technology developed during these experiments laid the groundwork for modern surgical robots.
The First Robotic Surgeons
The first actual use of a robot in human surgery occurred in 1985. Researchers used an adapted industrial robot arm called the PUMA 200 to perform a delicate brain biopsy. The robot was used because it could hold a needle with absolute steadiness, eliminating human hand tremors.
Following this success, other single-purpose robots were developed. A 2021 review in the Revista do Colegio Brasileiro de Cirurgioes notes that early robots like the PROBOT were designed specifically for prostate surgery, while the ROBODOC system was created in 1992 to help orthopedic surgeons carve bone with extreme precision during hip replacements.
These early machines were helpful, but they were limited. They could only perform very specific, pre-programmed tasks. The medical world needed a versatile robot that could act as a direct extension of a surgeon’s hands for a wide variety of operations.
The Race for the Modern Operating Room
In the 1990s, the race to build a multi-purpose surgical robot accelerated. A major breakthrough occurred with the invention of AESOP in 1994. AESOP was a voice-controlled robotic arm designed simply to hold and move a surgical camera. Before AESOP, a human assistant had to hold the camera during minimally invasive surgeries, and they would often become fatigued, causing the camera to shake.
Soon after, complete robotic systems emerged. The ZEUS robotic system made history in 2001 when it was used to perform the first transatlantic surgery. A surgeon sitting in New York successfully removed the gallbladder of a patient located in Strasbourg, France, using a high-speed fiber-optic connection.
However, it was the da Vinci Surgical System, approved by the FDA in 2000, that truly established robotic surgery as a standard medical practice. The da Vinci system solved several problems that earlier robots and traditional surgical methods could not.
How Robotic Surgery Actually Works
To understand why systems like the da Vinci became so popular, it helps to understand how they work. The system is built on a “master-slave” concept.
The surgeon sits at a computer console a few feet away from the patient. They look into a viewfinder that provides a high-definition, three-dimensional view of the inside of the patient’s body. The surgeon places their fingers into specialized controllers. When the surgeon moves their hands, the computer translates those movements in real-time to the robotic arms positioned over the patient.
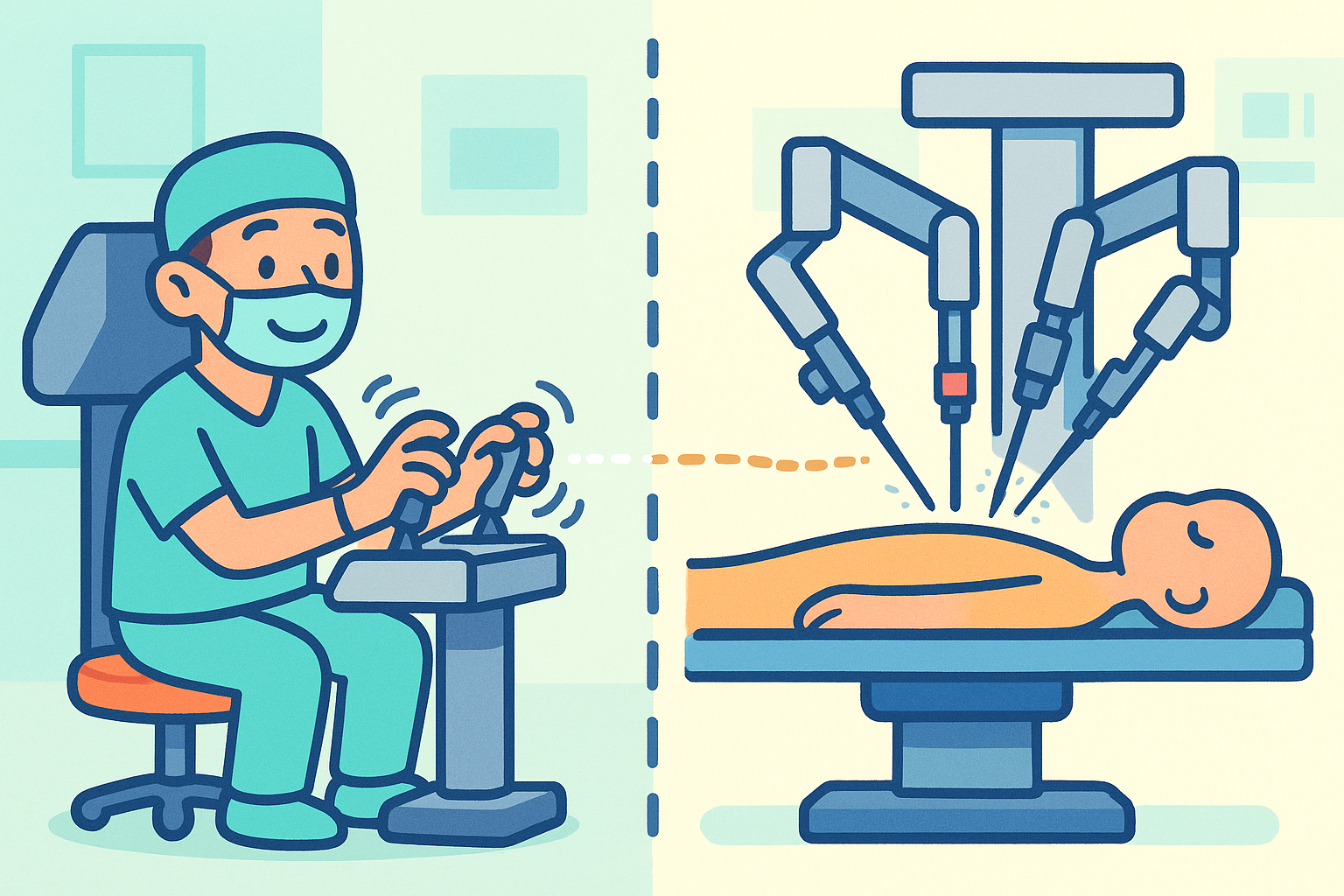
This setup provides several mechanical advantages:
- Tremor filtering: The computer smooths out the surgeon’s movements. If the surgeon’s hand shakes slightly, the robotic instrument remains perfectly still.
- Motion scaling: The surgeon can set the machine so that a large movement of their hand translates to a microscopic movement of the robotic instrument inside the patient.
- Degrees of freedom: Traditional laparoscopy (lap-uh-ROSS-kuh-pee), a type of minimally invasive surgery using rigid sticks, limits how a surgeon can move. Robotic instruments have mechanical wrists that mimic the human hand, allowing them to bend and rotate in tight spaces.
Comparing Surgical Methods
To see why doctors choose robotics, it helps to compare it to older methods.
| Feature | Open Surgery | Traditional Laparoscopy | Robotic-Assisted Surgery |
|---|---|---|---|
| Incision Size | Large (several inches) | Small (keyhole) | Small (keyhole) |
| Vision | Direct eyesight (2D) | Flat monitor (2D) | High-definition (3D) |
| Instrument Movement | Natural wrist movement | Rigid (straight sticks) | Fully wristed (flexible) |
| Surgeon Posture | Standing over patient | Standing, often awkward | Seated ergonomically |
What the Research Shows: Where Robots Shine
Robotic surgery is not necessary for every operation. However, research highlights specific medical fields where the technology provides clear benefits to patients.
Urology and Prostate Surgery
When the da Vinci system was first introduced, it was intended for heart surgery. However, urologists quickly realized it was the perfect tool for removing the prostate gland. The prostate is located deep inside the male pelvis, surrounded by sensitive nerves that control urinary and sexual function.
A 2022 review in The Urologic Clinics of North America highlights that robotic systems give surgeons the 3D vision and wristed instruments needed to carefully detach the prostate while preserving the surrounding nerves. Studies consistently show that robotic prostate surgery leads to less blood loss and shorter hospital stays compared to traditional open surgery.
Head and Neck Surgery (TORS)
Historically, removing tumors from the back of the throat or the base of the tongue required highly invasive procedures. Surgeons often had to split the patient’s lower jawbone just to reach the tumor, which led to long recoveries and difficulty swallowing or speaking.
This changed with Transoral Robotic Surgery (TORS). A 2020 paper in the Otolaryngologic Clinics of North America details how surgeons began using robotic arms to reach through the patient’s open mouth to remove tumors. Because the robotic arms are thin and flexible, they can navigate the natural curve of the airway. Research shows that patients who undergo TORS often recover their ability to swallow much faster than those who undergo traditional open neck surgery.
Spine Surgery
Operating on the spine requires extreme precision. A misplaced screw can cause nerve damage or paralysis. Related: Yoga vs. Physical Therapy for Back Pain: What Science Actually Says.
A 2020 review in the Journal of Medical Engineering & Technology examined the use of robotics in placing pedicle screws during spinal fusion surgeries. The research indicates that robotic guidance systems significantly increase the accuracy of screw placement. Additionally, because the robot guides the surgeon precisely, less intraoperative X-ray imaging is needed, which reduces radiation exposure for both the patient and the surgical team.
Common Questions About Robotic Surgery
Does the robot perform the surgery on its own?
No. The robot is completely passive. It only moves when the surgeon moves their hands at the control console. If the surgeon stops moving, the robot stops moving immediately.
Can the surgeon feel what the robot is touching?
Most current robotic systems lack haptic feedback (HAP-tik FEED-bak), which is the sense of touch or physical resistance. Instead, surgeons rely heavily on the highly magnified 3D visual cues to judge how much tension they are applying to tissues.
Is robotic surgery always better than traditional surgery?
Not always. For simple, straightforward procedures, traditional laparoscopic surgery is highly effective, faster to set up, and less expensive. Robotic surgery is most beneficial for complex procedures in tight, difficult-to-reach areas of the body.
Where The Science Is Still Evolving: Limitations and Future Tech
While robotic surgery has transformed modern medicine, it is not without drawbacks. The most significant limitation is cost. A single robotic system can cost millions of dollars to purchase, plus hundreds of thousands of dollars annually for maintenance and disposable instruments. This cost is often passed down through the healthcare system.
Furthermore, setting up the robot (called “docking”) takes time. For a simple procedure, the time spent preparing the robot might take longer than the surgery itself.
However, the future of this technology is advancing rapidly. A 2024 paper in Cirugia Espanola outlines how robotic surgery is driving the “digitalization” of the operating room. Future platforms are expected to include:
- Artificial Intelligence (AI): AI could analyze surgical video in real-time, warning the surgeon if they are getting too close to a hidden blood vessel.
- Augmented Reality: Surgeons may soon be able to overlay a patient’s MRI or CT scan directly onto their surgical view, essentially giving them “X-ray vision” during the operation. Related: How MRI Is Changing the Way Doctors Find Cancer.
- Miniaturization: Newer robots are becoming smaller and more flexible. Systems like the Medrobotics Flex System use snake-like robotic arms that can navigate winding pathways inside the body without making any external incisions.
The Bottom Line
Robotic surgery has come a long way from its origins as a military concept for battlefield medicine. Over the last 30 years, it has evolved into a highly precise tool that allows surgeons to perform complex operations through tiny incisions.
While the technology is expensive and requires specialized training, the research clearly shows that for certain procedures (like prostate removals, throat cancer surgeries, and spinal fusions), robotic assistance leads to less blood loss, fewer complications, and faster recovery times. As new competitors enter the market and artificial intelligence is integrated into these systems, surgical robots will likely become smaller, smarter, and more accessible in the years to come.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Origins of Robotic Surgery | Traces the history from military telepresence concepts to modern FDA-approved surgical robots. | PMID 30524184 |
| Evolution of Transoral Surgery | Details how robots enabled surgeons to remove throat tumors through the mouth, avoiding major jaw incisions. | PMID 30527249 |
| Robotic Spine Surgery | Shows that robotic assistance improves the accuracy of spinal screw placement and reduces radiation exposure. | PMID 32886014 |
| Digitalization of Surgery | Explores how modern robots are integrating data, AI, and augmented reality to improve surgical planning. | PMID 38801975 |
| History of Computer-Assisted Surgery | Reviews the transition from the first robotic brain biopsy in 1985 to the widespread use of the da Vinci system. | PMID 32169176 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply