It is normal for men to experience a gradual decline in testosterone as they age. In recent years, however, advertisements for “low T” clinics have surged. These clinics often promise that restoring testosterone will fix fatigue, build muscle, and improve mood.
While testosterone replacement therapy is a valid medical treatment, the science behind it is much more nuanced than a billboard ad might suggest. For some men, treatment is highly effective. For others, low testosterone is actually a symptom of a different health issue entirely.
This article breaks down what peer-reviewed research actually says about low testosterone, who truly benefits from treatment, and what risks are involved.
What Is Hypogonadism?
Doctors use the term Hypogonadism (hi-po-GO-nad-izm) to describe a condition where the body does not produce enough testosterone. This is not just a single low blood test result. A true diagnosis requires two things to be present at the same time: consistently low testosterone levels on morning blood tests and physical symptoms of that deficiency.

Symptoms often include a drop in sex drive, loss of muscle mass, fatigue, and mood changes. A 2014 review in The Lancet explains that hypogonadism can happen because the testicles fail to produce testosterone, or because the brain fails to send the right signals to the testicles.
What the Research Shows About Treatment Benefits
When a man has true hypogonadism, restoring his testosterone levels to a normal range can provide clear benefits. Scientists have studied these effects extensively.
Sexual Health and Desire
Sexual symptoms are the most common reason men seek testosterone treatment. A 2016 study in The Journal of Clinical Endocrinology and Metabolism looked at older men with low testosterone and found that treatment significantly improved their sexual desire and overall sexual activity.
However, the effects on erectile function are more complex. A 2024 study in The Journal of Clinical Endocrinology and Metabolism followed over 1,100 men for two years. The researchers found that while testosterone therapy improved sexual activity and desire, it did not significantly improve erectile function on its own. This suggests that erectile difficulties often have other causes, such as blood flow issues, which testosterone alone cannot fix.
Muscle, Bone, and Body Composition
Testosterone is an anabolic hormone, meaning it helps build tissue. A 2021 review in the Annual Review of Medicine confirms that testosterone treatment increases skeletal muscle mass and improves muscle strength.
It also plays a vital role in bone health. The same 2021 review highlights that testosterone therapy improves both the density and estimated strength of bones in the spine and hips. This is important because older men with low testosterone are at a higher risk for bone fractures.
Mood and Energy
Many men with low testosterone report feeling depressed or drained. Research shows that treatment can modestly improve depressive symptoms. However, it is not a cure for clinical depression. A 2024 review in American Family Physician notes that while some men experience better mood and energy, the results can vary from person to person.
The Obesity Connection: A Common Misunderstanding
One of the most important concepts in modern testosterone research is the relationship between weight and hormones. Extra body fat actively lowers testosterone levels.
Fat cells contain an enzyme that converts testosterone into estrogen. When a man carries excess weight, more of his testosterone is changed into estrogen. This signals the brain to slow down testosterone production.
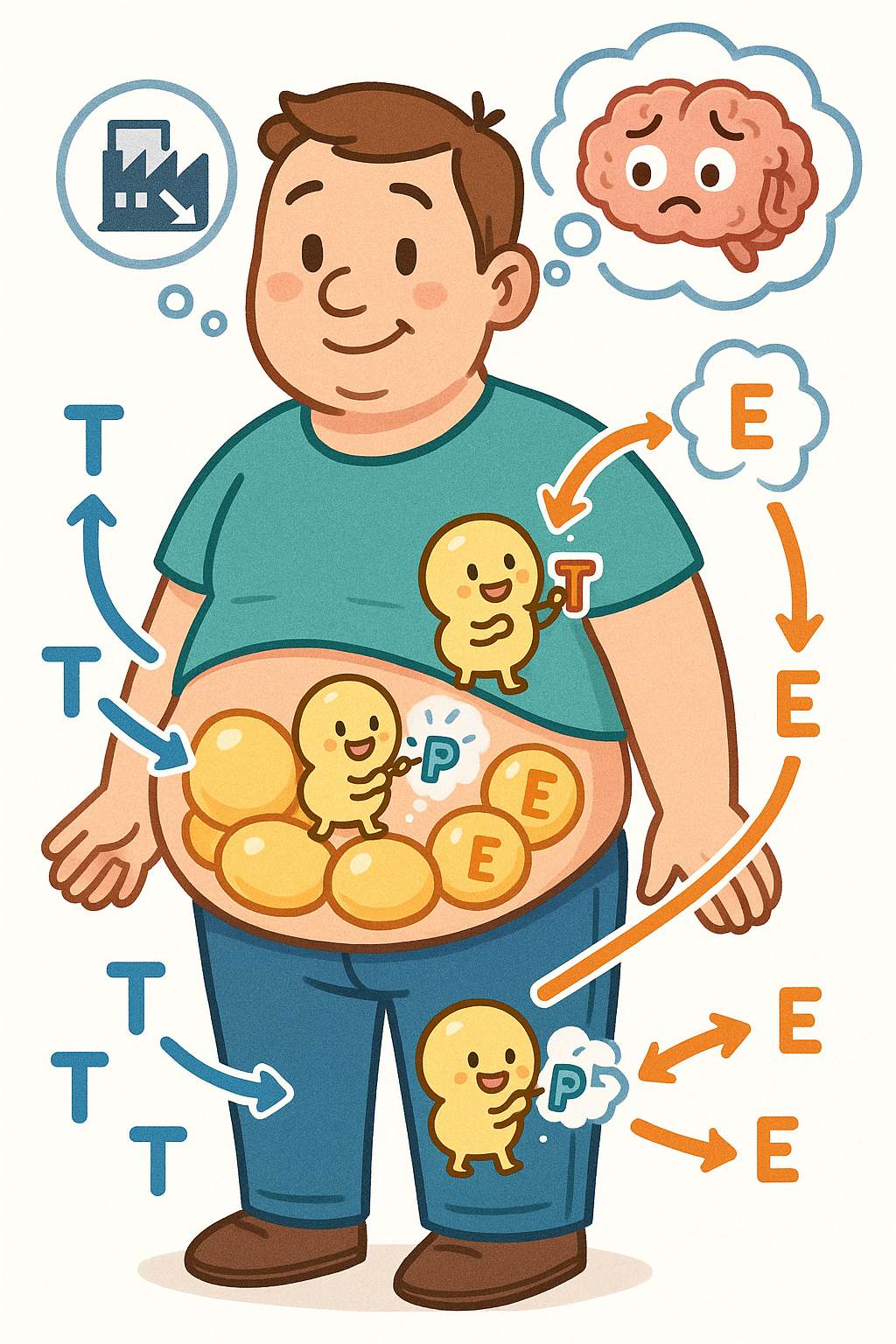
A 2025 study in The Journal of Clinical Endocrinology and Metabolism calls this “pseudo-hypogonadism.” The researchers emphasize that obesity is not a cause of permanent testicular failure. Instead, it is a reversible condition.
For men with obesity-related low testosterone, the most effective treatment is not a hormone prescription. It is weight loss. A 2015 review in Obesity Reviews confirms a bidirectional relationship: weight loss directly increases testosterone levels, and the more weight a man loses, the more his testosterone rises.
Related: GLP-1 Weight Loss Drugs: What Real-World Results Actually Show
Comparing True Hypogonadism and Obesity-Related Low T
| Feature | True Hypogonadism | Obesity-Related Low T |
|---|---|---|
| Root Cause | Testicular or brain signaling failure | Excess fat converting testosterone to estrogen |
| Reversible? | Usually no | Yes, with significant weight loss |
| Primary Treatment | Testosterone Replacement Therapy | Diet, exercise, or weight-loss interventions |
| Hormone Signaling | Abnormal | Normal, but suppressed by excess weight |
How This Might Work: The Fertility Problem
Understanding how the body regulates hormones explains why testosterone therapy causes infertility.
The brain and the testicles are in constant communication. The brain monitors testosterone levels in the blood. If levels are low, the brain releases signals to tell the testicles to make more testosterone and to produce sperm.
When a man takes external testosterone (via gels, injections, or patches), his blood levels rise. The brain senses this high level and stops sending signals to the testicles. As a result, the testicles stop producing their own testosterone and completely stop producing sperm.
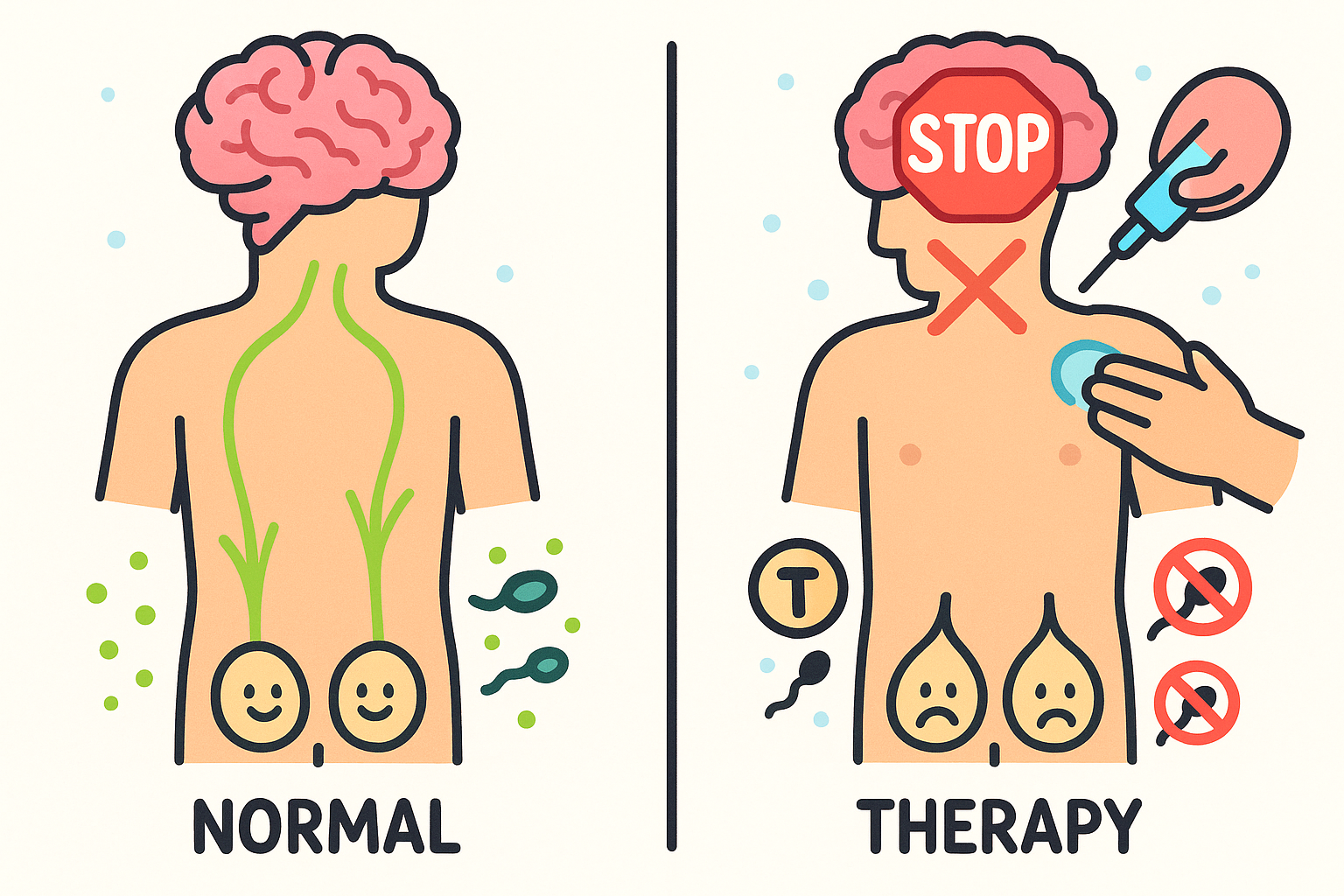
For men who want to have children, traditional testosterone therapy is not an option. A 2020 review in the International Journal of Molecular Sciences explains that alternative treatments must be used. Medications like clomiphene or human chorionic gonadotropin are often prescribed off-label to stimulate the body to make its own testosterone while preserving sperm production.
Where The Science Is Still Uncertain: Heart and Prostate Risks
For decades, doctors worried that testosterone therapy might cause prostate cancer or trigger heart attacks. Recent large-scale studies have provided clearer, though sometimes mixed, answers.
Prostate Cancer
The current scientific consensus is that testosterone therapy does not cause prostate cancer. A 2018 study in PloS One looked at thousands of men and found that testosterone treatment was not associated with an increased risk of developing aggressive prostate cancer, or any prostate cancer at all.
However, if a man already has prostate cancer, adding testosterone can act like pouring fuel on a fire. Because of this, doctors must carefully screen men for prostate issues before starting treatment and monitor them closely afterward.
Cardiovascular Health
The impact on the heart is still actively debated. A 2024 review in Health Technology Assessment analyzed multiple trials and found no difference in cardiovascular events between men taking testosterone and those taking a placebo in the short-to-medium term.
Conversely, a 2017 trial in JAMA used advanced imaging to look at the hearts of older men on testosterone therapy. They found that one year of treatment was associated with a greater increase in noncalcified plaque volume in the coronary arteries compared to a placebo. While this did not immediately cause heart attacks during the study, increased plaque is a known risk factor for heart disease over time.
Because of these mixed findings, men with a history of severe heart disease or recent heart attacks are generally advised to avoid testosterone therapy.
Who Needs Caution and Practical Guidance
Testosterone therapy requires careful medical supervision. It is not a medication that can be taken casually.
A 2025 review in the International Braz J Urol outlines several side effects that require strict monitoring:
- Erythrocytosis (uh-rith-ro-sy-TOE-sis) – This is a condition where the body produces too many red blood cells, making the blood abnormally thick. Thick blood increases the risk of blood clots and strokes. Doctors must regularly check a patient’s hematocrit (the percentage of red blood cells). If it gets too high, the testosterone dose must be lowered, or blood must be donated to thin it out.
- Sleep Apnea – Testosterone can worsen untreated obstructive sleep apnea. Men who snore heavily or stop breathing during sleep need to address their sleep apnea before starting therapy.
- Liver Function – While modern gels and injections are generally safe for the liver, older oral forms of testosterone were toxic to it. Regular blood tests ensure the liver remains healthy.
Related: Continuous Glucose Monitoring: What the Latest Science Says
A Note on Women and Testosterone
While usually discussed in the context of men’s health, testosterone is also a normal and essential hormone in women.
A 2025 study in Archives of Women’s Mental Health looked at peri- and postmenopausal women who experienced brain fog, low mood, and fatigue despite standard hormone therapy. The researchers found that adding a low, female-appropriate dose of transdermal testosterone significantly improved both mood and cognitive symptoms over four months.
Similarly, a 2025 review in Climacteric notes that while testosterone is currently only officially recommended for women to treat low sexual desire, emerging evidence suggests it plays important roles in other tissues throughout the female body.
The Bottom Line
Testosterone replacement therapy is a highly effective treatment for men with true, medically diagnosed hypogonadism. It can improve sexual desire, build muscle, strengthen bones, and boost overall quality of life.
However, it is not a magic cure for the natural aging process, nor is it the right solution for men whose low testosterone is caused by excess weight. For men with obesity, losing weight is the most scientifically sound way to restore hormone levels naturally.
Because testosterone therapy carries risks, including thickened blood and the potential to accelerate existing prostate issues, it requires ongoing medical monitoring. Anyone considering this treatment should have a detailed conversation with their doctor to weigh the clear benefits against the required safety checks.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Obesity and Low T | Extra weight suppresses testosterone. Weight loss effectively reverses this “pseudo-hypogonadism.” | PMID 40052430 |
| Sexual Function | Treatment improves sexual activity and desire, but does not reliably fix erectile function alone. | PMID 37589949 |
| Prostate Cancer Risk | Testosterone therapy does not increase the risk of developing aggressive prostate cancer. | PMID 29933385 |
| Heart Plaque | One year of treatment in older men increased noncalcified plaque volume in coronary arteries. | PMID 28241355 |
| Adverse Effects | The most common risk is thickened blood, requiring strict monitoring of red blood cell counts. | PMID 39908204 |
| Women’s Health | Low-dose treatment improved mood and cognition in postmenopausal women with persistent symptoms. | PMID 39283522 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply