Imagine your digestive tract as an exclusive, highly secure nightclub. The walls are solid, and the bouncers at the door have one job: let the good stuff (nutrients and water) inside and keep the troublemakers (bacteria, toxins, and undigested food) out.
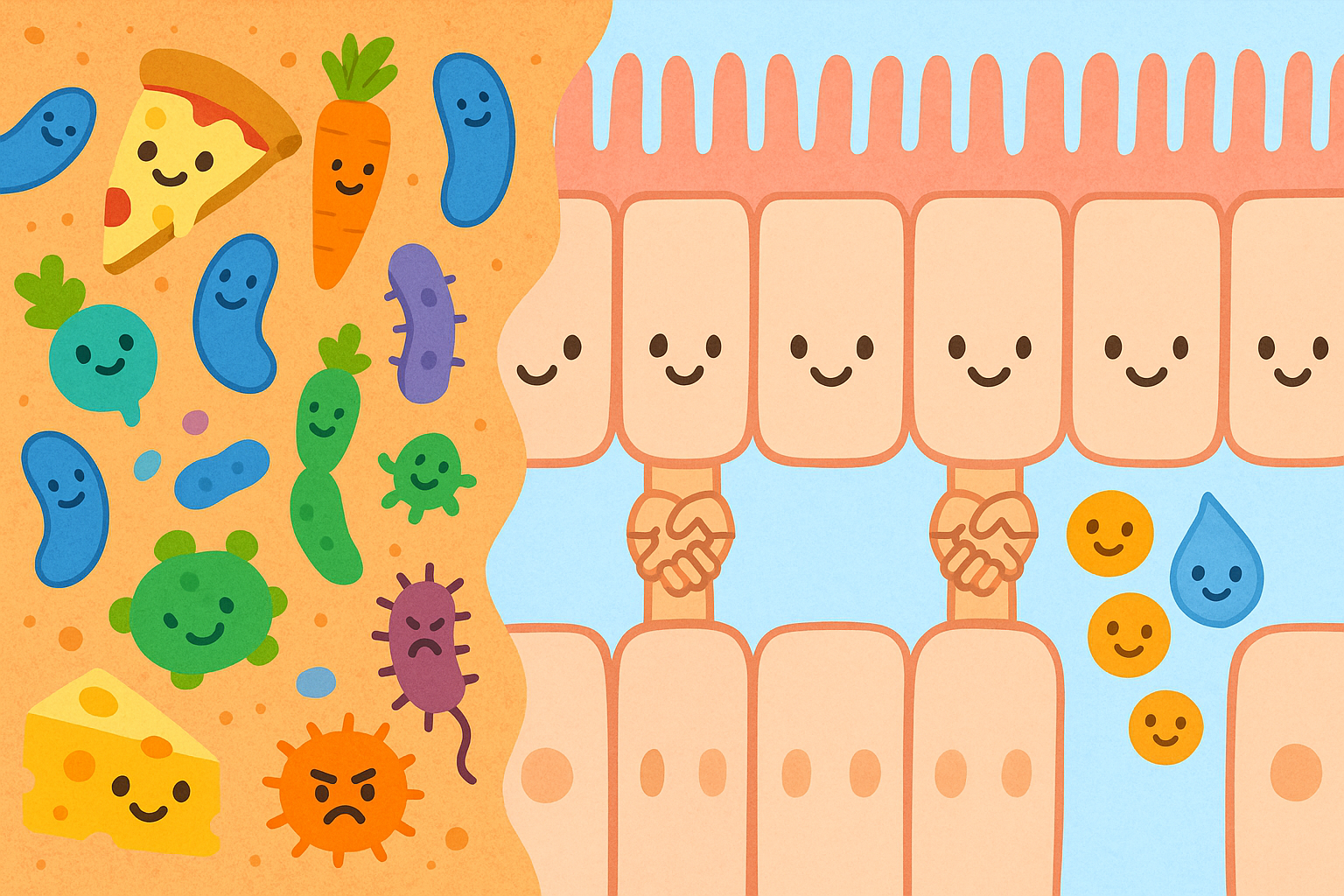
But what happens when the bouncers get tired or the doors break down?
This scenario is at the heart of a major medical debate. Leaky gut syndrome, scientifically known as increased intestinal permeability, happens when the tight gaps in the intestinal lining loosen. This allows bacteria and toxins to enter the bloodstream, triggering systemic inflammation that researchers are now linking to metabolic, autoimmune, and even brain disorders.
For years, “leaky gut” was a term primarily used in alternative medicine, often met with skepticism by traditional doctors. Today, however, gastroenterologists and researchers are studying it intensely under the name “intestinal permeability.” While they may disagree on the terminology, the science is clear: the integrity of your gut barrier plays a massive role in your overall health.
How the Gut Barrier Actually Works
To understand a leaky gut, we first have to understand a healthy one. The inside of your intestinal tract is technically part of the “outside” world. Food and bacteria travel through this tube, and your body must carefully decide what gets absorbed into your bloodstream.
Your intestinal barrier is surprisingly thin. It is made of a single layer of cells known as epithelial cells. These cells are glued together by complex protein structures called tight junctions (TITE JUNK-shuns). Tight junctions act as the bouncers, opening just enough to let tiny nutrients pass through, then snapping shut to block larger, harmful particles.
This physical barrier is supported by a thick layer of mucus and a vast community of trillions of microorganisms known as the gut microbiome. When this system is in balance, you are healthy. When the system breaks down, problems begin.
The Role of Dysbiosis and Toxins
When the balance of good and bad bacteria in your gut is disrupted, a condition called dysbiosis (dis-bye-OH-sis) occurs. Dysbiosis can damage the mucus layer and irritate the epithelial cells.
Certain bad bacteria produce toxins on their outer shells called lipopolysaccharides (lip-oh-poly-SACK-uh-rides), commonly referred to as LPS. According to a 2024 review in Internal and Emergency Medicine, when tight junctions loosen, LPS toxins “leak” into the bloodstream. The immune system recognizes these toxins as a massive threat and launches an inflammatory attack. This condition, known as metabolic endotoxemia, creates low-grade, chronic inflammation throughout the entire body.
Scientists have also identified a protein called zonulin (ZON-you-lin) that directly controls the tight junctions. A 2021 study in Frontiers in Immunology notes that certain triggers, including harmful bacteria and specific dietary proteins, can cause the body to release too much zonulin. When zonulin levels rise, the tight junctions stay open too long, leading to a leaky gut.

What the Research Shows
Modern research has moved beyond asking if the gut barrier can become permeable. Scientists are now investigating how this permeability contributes to various chronic diseases.
Autoimmune and Inflammatory Diseases
When foreign particles leak into the bloodstream, the immune system can become hyperactive. Over time, this constant state of high alert can confuse the immune system, causing it to attack the body’s own tissues.
Research has found strong links between increased intestinal permeability and several autoimmune conditions. Elevated levels of zonulin and LPS have been observed in patients with Type 1 diabetes, multiple sclerosis, and rheumatoid arthritis. In fact, a 2021 review in the International Journal of Environmental Research and Public Health highlights that in some cases, changes in intestinal permeability can be detected years before the actual clinical symptoms of autoimmune diseases like Crohn’s disease appear.
Metabolic Health and Liver Disease
The liver is the first organ to filter blood coming directly from the intestines. If the gut is leaky, the liver takes the brunt of the toxic hit.
A 2022 study in the International Journal of Molecular Sciences explains that the continuous flow of LPS toxins from a leaky gut into the liver drives inflammation and fat accumulation. This process is heavily linked to Non-Alcoholic Fatty Liver Disease (NAFLD) and insulin resistance. When the liver is constantly fighting off toxins, it struggles to manage blood sugar and fat storage properly. Related: Intermittent Fasting: What the Latest Science Actually Says
The Gut-Brain Connection
Can a leaky gut lead to a “leaky brain”? Emerging evidence suggests it might. The brain has its own protective shield called the blood-brain barrier. However, systemic inflammation originating in the gut can weaken this barrier.
A 2018 review in Microorganisms explores how gut-derived inflammatory signals and bacterial metabolites can cross a compromised blood-brain barrier. This neuroinflammation is currently being studied for its potential role in mood disorders, cognitive decline, and neurodevelopmental conditions. While the science here is still in its early stages, the connection between gut health and mental clarity is becoming increasingly evident.
Common Misunderstandings or Myths
Because the term “leaky gut” is so popular on the internet, it is surrounded by considerable misinformation. A 2024 review in Gastroenterology & Hepatology specifically addressed these myths to clarify what science actually supports.
Myth: Leaky gut syndrome is a standalone medical diagnosis.
Truth: In mainstream medicine, leaky gut is not currently recognized as a distinct disease. Instead, doctors and scientists view “intestinal permeability” as a mechanism or a symptom that contributes to other recognized diseases (like inflammatory bowel disease or celiac disease).
Myth: A simple blood or stool test can easily diagnose it.
Truth: Many commercial tests claim to definitively diagnose a leaky gut. However, researchers note that no single, validated clinical test currently exists for everyday medical practice. While scientists use complex tests (like the lactulose/mannitol ratio test) in research labs, the commercial tests sold to consumers are often unreliable.
Myth: A specific supplement can “cure” a leaky gut overnight.
Truth: The gut barrier is a complex, living ecosystem. While certain nutrients help repair the lining, no single pill can fix a leaky gut if a person continues to eat a poor diet, experience chronic stress, or misuse medications.
What Causes the Gut to Leak?
Research points to several modern lifestyle factors that compromise the “bouncers” at our intestinal doors.
- Dietary Choices: A Western diet high in saturated fats and highly refined carbohydrates is a major culprit. A 2021 study in Hepatology demonstrated that excessive fructose consumption specifically promotes leaky gut and endotoxemia by causing oxidative stress that degrades tight junction proteins.
- Medications: Overuse of non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can physically damage the intestinal lining. Additionally, proton pump inhibitors (PPIs) alter stomach acid, which can lead to bacterial overgrowth further down the digestive tract.
- Alcohol: Heavy alcohol consumption is a well-documented toxin to the intestinal lining, actively breaking down tight junctions and feeding harmful bacteria.
- Stress: Chronic psychological and physical stress reduces blood flow to the gut and alters immune responses, making the barrier more vulnerable to damage.
Practical Guidance: How to Support Your Gut Barrier
If lifestyle factors can damage the gut barrier, they can also help repair it. The intestinal lining replaces its cells every few days, meaning it has a remarkable capacity to heal if given the right tools.
According to a 2022 review in the International Journal of Molecular Sciences, several dietary interventions show promise in maintaining and repairing the intestinal barrier:
1. Increase Dietary Fiber
Fiber is not just for digestion. Beneficial gut bacteria eat soluble fiber and produce short-chain fatty acids (SCFAs), specifically one called butyrate. Butyrate is the primary energy source for your intestinal cells. It actively helps rebuild tight junctions and reduces local inflammation.
2. Focus on Healthy Fats and Polyphenols
The Mediterranean diet, which is rich in omega-3 fatty acids (from fish) and polyphenols (from olive oil, berries, and green tea), has been shown to support a healthy microbiome and protect tight junctions from oxidative stress.
3. Consider Specific Amino Acids
Glutamine is an amino acid that serves as a major fuel source for the cells lining your intestines. Several studies indicate that glutamine supplementation can help restore tight junction function, especially after physical stress or illness.
4. Probiotics and Prebiotics
Certain strains of bacteria, particularly from the Lactobacillus and Bifidobacterium families, have been shown to strengthen the gut barrier and crowd out toxin-producing bacteria. Prebiotics (the food that feeds these good bacteria) are equally vital. Related: What Science Actually Says About Fecal Transplants for Gut Health
Where The Science Is Still Uncertain
While the existence of intestinal permeability is undeniable, the classic “chicken or the egg” question remains. Scientists are still debating whether a leaky gut causes systemic diseases, or if systemic diseases cause the gut to become leaky.
For example, does a leaky gut cause obesity by letting inflammation-triggering toxins into the blood? Or does the poor diet that leads to obesity also happen to damage the gut lining? In reality, it is likely a vicious cycle where each factor worsens the other.
Common Questions About Leaky Gut
Is leaky gut a real medical diagnosis?
Not officially. While “intestinal permeability” is a heavily researched scientific phenomenon, “leaky gut syndrome” is not currently recognized as a standalone diagnosis in standard medical manuals. It is viewed as an underlying mechanism of other diseases.
What are the symptoms of a leaky gut?
Because the toxins leak into the bloodstream, symptoms are often systemic rather than just digestive. They can include chronic fatigue, joint pain, brain fog, unexplained skin rashes, and widespread inflammation, alongside traditional digestive issues like bloating.
Can artificial sweeteners cause a leaky gut?
Emerging research suggests that some artificial sweeteners may negatively alter the gut microbiome, reducing beneficial bacteria and promoting strains that disrupt the intestinal barrier, though more human studies are needed to confirm the exact impact.
The Bottom Line
The concept of “leaky gut” is no longer just an alternative health buzzword. There is robust, peer-reviewed evidence showing that the intestinal barrier can become compromised, allowing toxins and bacteria to enter the bloodstream. This “intestinal permeability” drives chronic inflammation and is closely linked to autoimmune, metabolic, and neurological conditions.
While we do not yet have a simple pill or a perfect diagnostic test, the science clearly shows that our daily choices matter. By limiting excess fructose, alcohol, and unnecessary medications, and by embracing a diet rich in fiber and healthy fats, you can support the “bouncers” in your gut and keep your body’s internal borders secure.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Fructose and Permeability | High fructose intake causes protein damage to tight junctions, leading to gut leakiness and liver fibrosis. | PMID 30959577 |
| Autoimmunity Links | Disruption of the epithelial barrier and dysbiosis are strongly linked to autoimmune diseases like Type 1 diabetes and multiple sclerosis. | PMID 33968085 |
| Dietary Prevention | Diets high in fiber and specific amino acids like glutamine can improve barrier function and restrict bacterial invasion. | PMID 35328624 |
| Leaky Gut Myths | While intestinal permeability is real, “Leaky Gut Syndrome” lacks validated diagnostic tests and is not a formal standalone diagnosis. | PMID 39193076 |
| Gut-Brain Axis | Intestinal barrier disruption and systemic inflammation can compromise the blood-brain barrier, potentially influencing neurological disorders. | PMID 30340384 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.



Leave a Reply