Introduction
If you follow health news or visit a dermatology clinic, you have likely heard of Platelet-Rich Plasma (PRP) therapy. It is used for everything from treating sports injuries to regrowing hair and rejuvenating skin. But what is it exactly, and does the science support the claims?
At its core, PRP is a treatment that uses your own blood to encourage tissue repair. By isolating specific healing components in your blood and injecting them directly into injured or aging tissues, doctors aim to speed up the body’s natural repair process.
Research shows that PRP can be effective for certain conditions, particularly mild to moderate joint pain and specific types of hair loss. However, it is not a magic cure. The results can vary widely from person to person, and scientists are still trying to figure out the exact “recipe” that works best. In this article, we will break down what the latest peer-reviewed research actually says about PRP, where it works best, and where the evidence is still lacking.
How This Might Work: The Biology of PRP
To understand PRP, it helps to understand what is in your blood. Human blood is mostly made of a liquid called plasma. Floating in this plasma are red blood cells, white blood cells, and platelets.
- Platelets (PLAYT-lets) are tiny cell fragments best known for helping blood clot when you get a cut.
- Growth factors (GROTH fak-ters) are special proteins stored inside platelets.
Think of platelets as the body’s emergency response team. When tissue is damaged, platelets arrive at the scene and release growth factors. These growth factors act like signal flares, calling in other cells to repair damaged tissue, build new blood vessels, and reduce inflammation.

A 2020 review in the International Journal of Molecular Sciences explains that PRP therapy works by capturing these platelets and concentrating them. A doctor draws a small amount of your blood and places it in a machine called a centrifuge. This machine spins the blood rapidly, separating the platelets from the red and white blood cells. The concentrated platelets are then injected directly into the target area, delivering a high dose of growth factors exactly where they are needed.
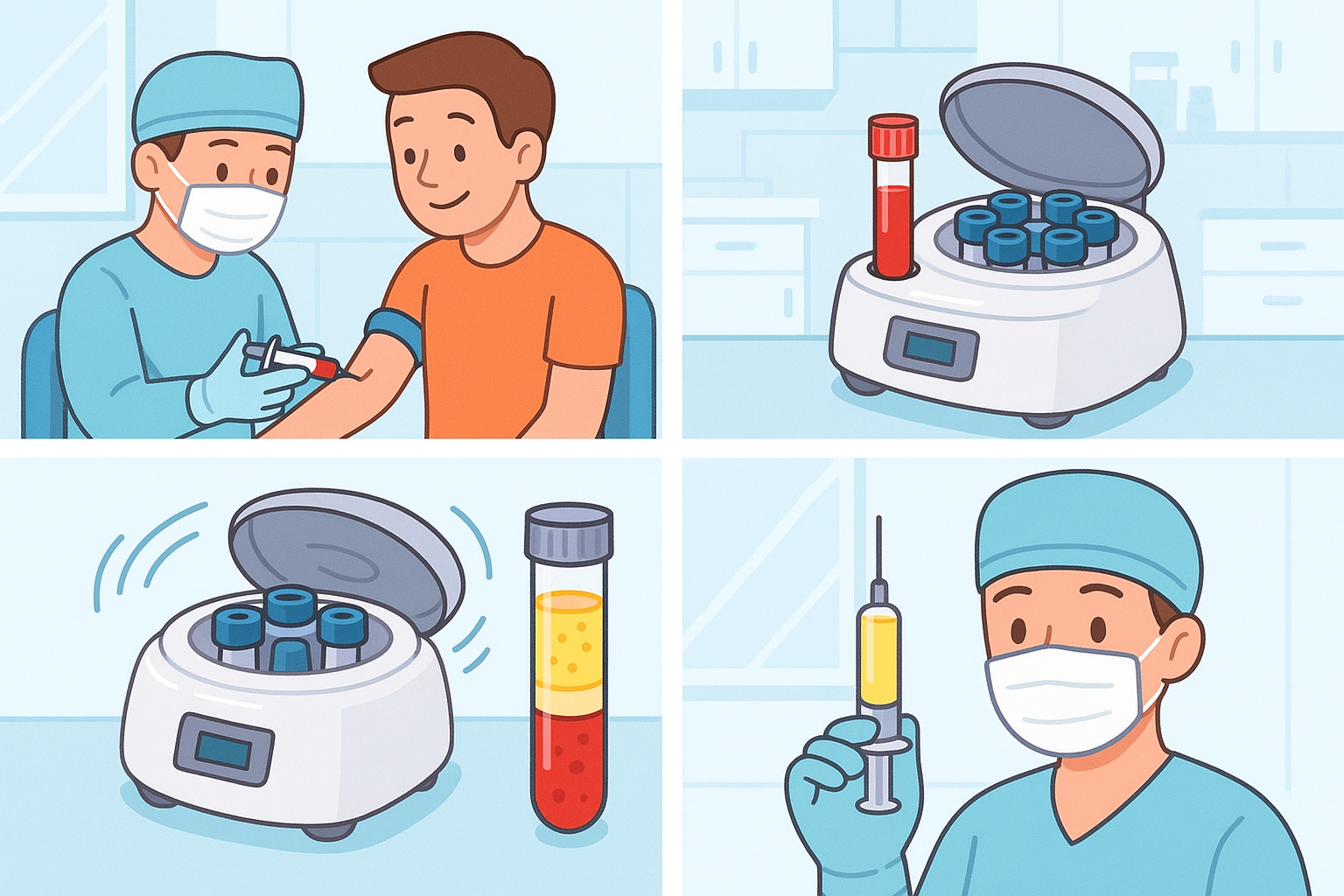
Because PRP uses your own blood, it is called an autologous (aw-TOL-uh-gus) treatment. This means there is a very low risk of allergic reaction or rejection.
What the Research Shows: Hair Loss
One of the most popular uses for PRP is treating hair loss, specifically androgenetic alopecia (an-dro-jen-ET-ik al-oh-PEE-sha). This is the medical term for common male or female pattern baldness, which is closely tied to hormones and genetics. For readers exploring how hormones impact the body, you might also find our guide on What Science Actually Says About Low Testosterone Treatment helpful.
Research indicates that PRP is quite effective for this type of hair loss. A 2020 systematic review in the International Journal of Molecular Sciences analyzed multiple clinical trials comparing PRP to standard treatments like minoxidil. The review found that 84% of the studies reported a positive effect on hair regrowth.
According to a 2021 review in Dermatologic Clinics, PRP helps hair loss by:
- Prolonging the growing phase of the hair cycle.
- Increasing the thickness of existing hair shafts.
- Improving blood supply to the hair follicles.
While the results are promising, researchers note that PRP works best for people with mild to moderate hair loss rather than complete baldness. It also requires maintenance. Most clinical protocols involve three to four initial monthly sessions, followed by maintenance treatments a few times a year.
What the Research Shows: Joint Pain and Osteoarthritis
Osteoarthritis (os-tee-oh-ar-THRY-tis) happens when the protective cartilage that cushions the ends of your bones wears down over time. It commonly affects the knees, hips, and hands. While many people turn to physical therapy to manage joint issues (a topic we cover in Yoga vs. Physical Therapy for Back Pain: What Science Actually Says), injections are another common medical option.
Multiple studies have tested PRP against hyaluronic acid (a common lubricating gel injected into joints) for osteoarthritis.
A 2017 review in Current Rheumatology Reports looked at 15 clinical trials for knee osteoarthritis and three for hip osteoarthritis. The researchers concluded that PRP is safe and often provides better symptom relief than hyaluronic acid for up to 12 months.
Similarly, a 2024 study in Regenerative Medicine investigated combining PRP with hyaluronic acid for knee osteoarthritis. The researchers found that using both treatments together offered better pain relief and improved physical function compared to using either treatment alone.
PRP has also been tested on smaller joints. A 2023 trial in the Journal of Cranio-Maxillo-Facial Surgery looked at 70 patients with osteoarthritis of the jaw (the TMJ joint). The patients who received PRP had greater improvements in pain and mouth opening compared to those who received hyaluronic acid.
Who Benefits Most?
The evidence suggests that PRP works best for younger patients and those with early-stage, mild-to-moderate osteoarthritis. It appears to reduce pain and improve function, but there is currently no strong evidence that PRP can actually regrow lost cartilage in humans.
What the Research Shows: Skin Rejuvenation and Dermatology
Dermatologists frequently use PRP for anti-aging and skin repair. When injected into the skin, the growth factors in PRP stimulate cells to produce more collagen and elastin, which give skin its firmness and bounce.
A 2024 study in Skin Research and Technology reviewed 11 clinical trials involving 382 patients. The researchers found that after one to three sessions, patients saw visible improvements in skin texture, pore size, and wrinkle reduction.
PRP is also being studied for melasma (muh-LAZ-muh), a condition that causes dark, discolored patches on the skin. A 2021 study in the Journal of Cosmetic Dermatology highlighted that a specific growth factor in PRP (called TGF-beta) helps block the pathways that produce excess skin pigment.
Furthermore, PRP is frequently combined with microneedling. A 2017 review in Cutis found that applying PRP during microneedling improves cosmetic outcomes and speeds up healing compared to microneedling alone.
What the Research Shows: Tendons and Fasciitis
Tendon injuries heal very slowly because tendons generally have a poor blood supply. Because PRP delivers concentrated healing factors directly to the tissue, it is frequently used for sports injuries.
However, the results here are more mixed than with hair loss or osteoarthritis.
- Rotator Cuff Tears: A 2024 randomized controlled trial in the Journal of Orthopaedic Surgery and Research tested PRP injections (with and without Vitamin C) for partial shoulder tears. Both groups experienced significant pain reduction and improved function over three months.
- Plantar Fasciitis: A 2024 meta-analysis in Foot & Ankle International compared PRP to shock wave therapy for heel pain. While PRP provided statistically better pain reduction, the researchers noted the difference was small and might not be highly noticeable to the average patient.
Emerging Uses: Reproductive Health
Scientists are also exploring PRP in fertility treatments, though this research is still in its early stages.
For some women undergoing in vitro fertilization (IVF), the lining of the uterus (the endometrium) does not grow thick enough to support a pregnancy. A 2025 review in the Archives of Gynecology and Obstetrics looked at using PRP to help thicken this lining. The review found that infusing PRP into the uterus may enhance thickness and improve pregnancy rates.
Similarly, a 2021 review in the Journal of Assisted Reproduction and Genetics noted that injecting PRP into the ovaries might help women with poor ovarian reserve. While these initial findings are positive, researchers stress that PRP in reproductive medicine is still considered experimental until larger trials are completed.
Where The Science Is Still Uncertain: The “Recipe” Problem
If you read through PRP research, you will quickly notice a core tension: some studies show excellent results, while others show no benefit at all. Why do scientists disagree?
The main reason is the lack of standardization. Currently, there is no universal “recipe” for making PRP.

A 2009 paper in Trends in Biotechnology explains that depending on the specific machine used, the speed of the spin, and the time spent spinning, the final PRP product can look completely different.
For example, some preparation methods leave a high number of white blood cells (leukocytes) in the mixture, while others remove them entirely. Some scientists believe white blood cells help fight infection and aid healing, while others argue they cause unnecessary inflammation that slows down recovery.
Furthermore, a 2020 review in the International Journal of Molecular Sciences points out that red blood cell contamination in PRP can actually be toxic to tissues and cause severe inflammation. Until the medical community agrees on a standard preparation method for specific conditions, patient results will likely remain somewhat unpredictable.
Common Questions About PRP Therapy
Is PRP safe?
Yes. Because PRP is made from your own blood, the risk of an allergic reaction or disease transmission is incredibly low. The most common side effects are temporary pain, swelling, or bruising at the injection site.
How long does it take to see results?
PRP is not a quick fix. Because it relies on growing new cells and repairing tissue, it typically takes several weeks to a few months to see noticeable improvements in hair growth, joint pain, or skin texture.
Is PRP a permanent cure?
No. For degenerative conditions like osteoarthritis or genetic conditions like pattern baldness, PRP manages symptoms but does not cure the underlying disease. Most patients require maintenance treatments to sustain their results.
The Bottom Line / Takeaways
- What we know: Platelet-Rich Plasma (PRP) is a safe, low-risk therapy that uses concentrated healing factors from your own blood.
- Strongest evidence: The most consistent positive results are seen in treating male and female pattern hair loss, and mild-to-moderate knee osteoarthritis.
- What remains uncertain: Because preparation methods vary wildly between clinics, the quality and effectiveness of the PRP you receive can be unpredictable.
- Confidence level: We have moderate to high confidence in PRP’s safety and short-term effectiveness for specific conditions, but low confidence in its ability to provide permanent cures or regrow lost joint cartilage.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Hair Loss (Alopecia) | 84% of analyzed trials showed positive effects on hair density and thickness compared to controls. | PMID 32295047 |
| Knee & Hip Osteoarthritis | PRP safely provides symptomatic pain relief up to 12 months, often outperforming hyaluronic acid. | PMID 28386761 |
| Skin Rejuvenation | 1 to 3 sessions significantly improve skin texture, pore size, and wrinkle reduction. | PMID 38650371 |
| Rotator Cuff Tears | PRP injections significantly reduced pain and improved function over a 3-month period. | PMID 39044241 |
| PRP Preparation Methods | Highlights that differences in centrifuges and cell counts cause vast differences in clinical outcomes. | PMID 33096812 |
| IVF / Thin Endometrium | Intrauterine PRP may improve endometrial thickness and pregnancy rates, though still experimental. | PMID 40504243 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply