Imagine your eye is like a digital camera. The retina is the sensor at the back that captures the image. When someone has diabetes, chronic high blood sugar can slowly damage the tiny blood vessels supplying power to that sensor. Over time, this damage can lead to blurry vision or even blindness.
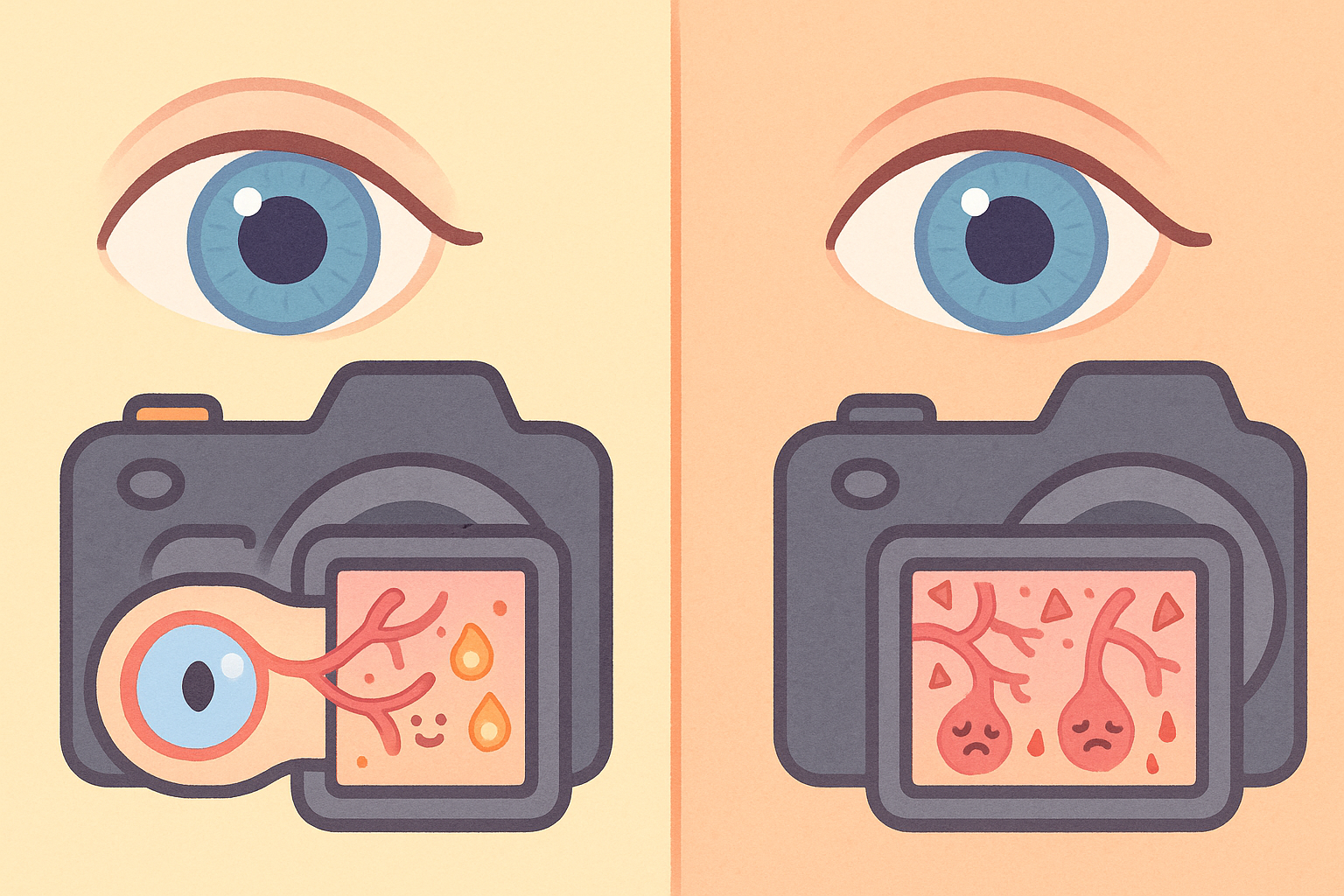
This condition is known as diabetic retinopathy (dye-uh-BET-ik ret-ih-NOP-uh-thee), which simply means disease of the retina caused by diabetes. For decades, it has been a leading cause of vision loss in adults.
However, there is excellent news. Modern science shows that severe vision loss from diabetes is largely preventable. By understanding how the disease works, controlling metabolic health, and getting the right screening, most people with diabetes can protect their vision for life.
This article breaks down what the latest research says about how diabetic eye disease develops, why regular screening is critical, and what treatments actually work.
How Diabetes Affects the Eyes
To understand how to prevent diabetic eye disease, it helps to know how it starts.
When blood sugar remains high over a long period, it damages the walls of the tiny blood vessels in the retina. A 2021 review in Clinical & experimental ophthalmology explains that this damage progresses in a few specific ways:
1. Vessel Leaks: The weakened blood vessels begin to leak fluid and fats into the retina.
2. Swelling: This fluid buildup can cause diabetic macular edema (dye-uh-BET-ik MAK-yoo-ler uh-DEE-muh), or DME. The macula is the center part of the retina responsible for sharp, straight-ahead vision. When it swells, vision becomes blurry.
3. Oxygen Starvation: As vessels become blocked, the retina is starved of oxygen.
4. Abnormal Growth: To survive, the oxygen-starved retina produces a distress signal called VEGF (VASH-yoo-ler en-doh-THEE-lee-uhl growth fak-ter). VEGF tells the eye to grow new blood vessels. Unfortunately, these new vessels are fragile, bleed easily into the eye, and can cause scar tissue to form.
Interestingly, the damage is not just about blood vessels. A 2021 study in Diabetologia found that diabetes also causes early damage to the actual nerve cells in the retina. This means diabetic eye disease is both a vascular (blood vessel) and neural (nerve) condition.
Related: Intermittent Fasting: What the Latest Science Actually Says
What the Research Shows About Prevention
The most effective way to prevent vision loss is to stop the disease from progressing to the later, more severe stages. Research highlights three main pillars of prevention: strict screening, metabolic control, and managing related conditions.
The Success of Routine Screening
Diabetic eye disease is often completely silent in its early stages. By the time a person notices blurry vision, the damage is usually advanced. Because of this, routine eye exams are the absolute most important preventive step.

When populations are screened regularly, blindness rates plummet. A 1997 study in Acta ophthalmologica Scandinavica followed diabetic patients in Iceland over four years. Because these patients received regular eye screenings and prompt laser treatment when needed, the rate of new legal blindness in the group was literally zero.
Similarly, a 2014 study in The British journal of ophthalmology reviewed the Scottish National Diabetic Retinopathy Screening Programme. They found that implementing a nationwide screening system successfully caught thousands of asymptomatic cases of macular swelling, allowing for early treatment and saving countless years of sight.
Controlling the Whole Body
Because diabetic retinopathy is an eye complication of a whole-body disease, systemic health matters.
The famous ACCORD Eye Study, detailed in a 2014 review in Ophthalmology, tested how different medical therapies affected eye disease progression in type 2 diabetes. The researchers found that intensive blood sugar control significantly slowed the progression of retinopathy.
They also found that adding a specific cholesterol-lowering medication (fenofibrate) to a standard statin reduced the progression of eye disease. However, the study noted that extremely tight blood sugar control carries other medical risks, so patients must work with their doctors to find a safe, balanced target.
Obesity and Dry Eye Connections
Recent science has also uncovered surprising links between diabetes and other eye conditions.
A 2024 review in Clinical obesity highlights that obesity independently increases the risk of diabetic retinopathy, cataracts, and glaucoma. The excess fat tissue produces inflammatory signals that can worsen eye health.
Furthermore, people with diabetes frequently suffer from severe dry eye. A 2021 study in Investigative ophthalmology & visual science and a 2023 review in Critical reviews in microbiology suggest that high blood sugar alters the natural bacteria living on the surface of the eye. This bacterial imbalance promotes inflammation and reduces tear quality, explaining why diabetic patients often experience chronic eye irritation.
Common Questions About Diabetic Eye Disease
When should I get my eyes checked?
According to a 2020 synopsis in Indian journal of ophthalmology and global guidelines, people with Type 2 diabetes should get a comprehensive eye exam right when they are diagnosed, because the disease may have been silently present for years. People with Type 1 diabetes should typically have their first exam within five years of diagnosis. After that, annual exams are the standard rule for everyone.
Can my vision improve if I lower my blood sugar?
If your vision is blurry simply because your blood sugar is currently spiking, it will often return to normal once your glucose levels stabilize. However, if the blurriness is caused by physical damage to the blood vessels (like leaking fluid or bleeding), you will likely need medical treatment to restore or protect your sight.
Do I still need an eye exam if my vision is perfect?
Yes. The early stages of diabetic retinopathy do not cause any vision changes. An eye doctor can see the tiny leaks and microaneurysms long before they reach the center of your vision.
Practical Guidance: How Doctors Treat It
If screening detects diabetic eye disease, ophthalmologists have several effective tools to stop it in its tracks.
Anti-VEGF Injections
As mentioned earlier, the damaged retina produces a protein called VEGF to grow new blood vessels. Doctors can inject a medicine directly into the eye that blocks VEGF. A 2017 review in Eye (London, England) notes that anti-VEGF therapy is now the standard of care for treating diabetic macular edema. It reduces swelling and frequently improves vision. While the idea of an eye injection sounds frightening, the eye is numbed, and the procedure is usually quick and painless.
Laser Therapy
Before injections existed, lasers were the main treatment. Today, they are still highly effective. Doctors use lasers to seal leaking blood vessels or to treat the outer edges of the retina. A 1993 review in Eye (London, England) explains that “scatter” laser treatment reduces the retina’s demand for oxygen, which stops the growth of abnormal, bleeding blood vessels.
Vitrectomy Surgery
If abnormal blood vessels bleed heavily into the center of the eye, or if they create scar tissue that pulls on the retina, surgery may be required. A 1992 review in Survey of ophthalmology details how a vitrectomy (vih-TREK-tuh-mee) involves carefully removing the blood-filled gel from the eye and peeling away scar tissue to flatten the retina back into place.
| Treatment Type | How It Works | Best Used For |
|---|---|---|
| Anti-VEGF Injections | Blocks the signal that causes swelling and abnormal vessel growth | Diabetic macular edema (swelling) and some abnormal vessel growth |
| Laser Therapy | Seals leaks and reduces the retina’s need for oxygen | Severe retinopathy to prevent retinal detachment and bleeding |
| Vitrectomy | Surgically removes blood and scar tissue from inside the eye | Advanced disease with persistent bleeding or retinal traction |
How This Might Work in the Future
Scientists are actively looking for ways to treat diabetic eye disease earlier and less invasively.
Recent animal studies point toward the immune system. A 2024 study in Journal of neuroinflammation found that expanding specific immune cells (Regulatory T cells) in mice prevented early retinal degeneration by calming inflammation.
Another avenue is targeting specific cellular receptors. A 2023 study in Cells showed that activating a receptor called RXR with a special eye drop improved lipid metabolism and preserved retinal function in diabetic mice. While these treatments are not yet ready for humans, they show that future therapies might focus on reducing inflammation rather than just blocking blood vessel growth.
The Bottom Line
Diabetic eye disease is a serious condition, but it is no longer a guaranteed path to vision loss. The science is very clear on a few key points:
- Screening is non-negotiable. Getting a dilated eye exam every year allows doctors to catch damage while it is still entirely treatable.
- Metabolic control protects the eyes. Managing blood sugar, blood pressure, and cholesterol slows the progression of the disease.
- Treatments work well. If you do develop macular swelling or abnormal blood vessels, modern treatments like anti-VEGF injections and laser therapy are highly effective at preserving sight.
The most important takeaway is that you do not have to wait for symptoms to appear. By staying proactive with your healthcare team, you can keep your eyes healthy for a lifetime.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Screening Success | An active annual screening program in Iceland resulted in zero new cases of legal blindness over a four-year period. | PMID 9253967 |
| Systemic Therapies | The ACCORD Eye Study showed that tight blood sugar control and specific lipid therapies slow the progression of diabetic retinopathy. | PMID 25459462 |
| Pathophysiology | A comprehensive review confirming that chronic hyperglycemia drives hypoxia, leading to VEGF release and vision-threatening complications. | PMID 33438363 |
| Dry Eye Link | Diabetic patients with dry eye show significant imbalances in their ocular surface bacteria compared to healthy individuals. | PMID 34524384 |
| Future Treatments | Expanding Regulatory T cells in diabetic mice prevented early retinal neurodegeneration and inflammation. | PMID 39716335 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen or changing your diabetes management plan.




Leave a Reply