Introduction
Vitamin E is often marketed as a skin-saving, heart-protecting, anti-aging super-nutrient. If you walk down the supplement aisle, you might assume that taking a daily Vitamin E capsule is a simple insurance policy for your health. However, the scientific reality is much more complex.
While Vitamin E is absolutely essential for human survival, acting as a bodyguard for your cells against damage, decades of research have revealed a confusing pattern: people who eat foods rich in Vitamin E tend to be healthier, but people who take Vitamin E pills often don’t see the same benefits. In some cases, high-dose supplements may even carry risks.
This article breaks down exactly what Vitamin E does in your body, why it is critical for your liver and cell membranes, and why scientists caution against treating it like a generic cure-all.
What Is Vitamin E?
To understand Vitamin E, you first have to understand that it is not a single molecule. It is a family of eight related fat-soluble compounds found in nature: four tocopherols (toe-KOFF-er-alls) and four tocotrienols (toe-koe-TRY-en-ols).
Among these, alpha-tocopherol is the form most recognized and used by the human body. Your liver contains a specific transport protein that preferentially selects alpha-tocopherol to send back into your bloodstream, while largely filtering out the others to be excreted.
The Bodyguard for Fats
Vitamin E’s primary job is to function as a lipid-soluble antioxidant. “Lipid-soluble” means it dissolves in fat. This is crucial because every cell in your body is enclosed in a membrane made largely of fats (lipids). These fats are vulnerable to “rusting” or oxidation caused by free radicals, unstable molecules produced by metabolism, pollution, and UV light.
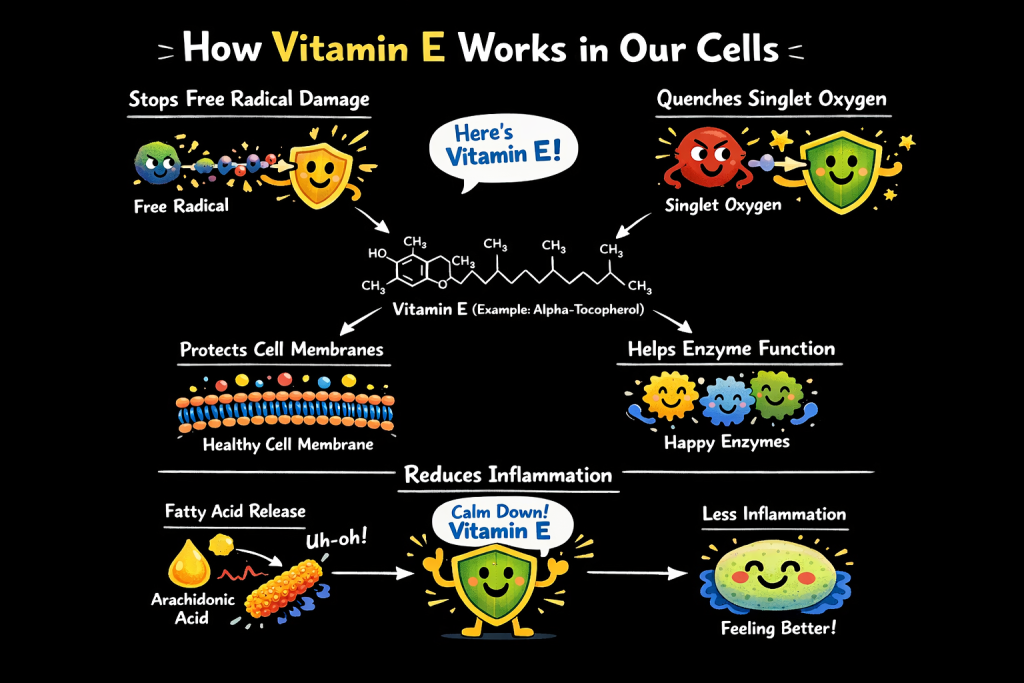
Think of your cell membranes like a butter wrapper. If left out in the sun and air, fats turn rancid. Vitamin E embeds itself inside your cell membranes to stop this “rancidity” (lipid peroxidation) before it destroys the cell.
What the Research Shows
Scientific research on Vitamin E is a tale of two extremes: it is highly effective for specific deficiencies and liver conditions, but surprisingly disappointing for general disease prevention.
1. Liver Health and NASH
One of the strongest evidence-based uses for Vitamin E is in treating a condition called Nonalcoholic Steatohepatitis (NASH), a severe form of fatty liver disease.
A landmark study in The New England Journal of Medicine found that Vitamin E supplementation (800 IU daily) was significantly better than a placebo at improving liver histology in non-diabetic adults with NASH. It helped reduce liver inflammation and fat buildup. However, because high doses carry risks, this treatment is generally supervised by a doctor.
Related: Can Supplements Slow Down Your Liver’s Aging Clock?
2. The Link Between PUFAs and Vitamin E Needs
Interestingly, your need for Vitamin E may depend on your diet. A 2015 review in The British Journal of Nutrition highlighted that Vitamin E requirements rise as you consume more polyunsaturated fatty acids (PUFAs), such as those found in vegetable oils (soybean, corn, sunflower). Because PUFAs are chemically unstable and prone to oxidation, the body requires more Vitamin E to protect them. The researchers estimated that for every gram of PUFA consumed, a small amount of additional Vitamin E is needed to prevent oxidative damage.
3. Heart Disease and Cancer Prevention
For decades, scientists hoped Vitamin E supplements would prevent heart attacks and cancer. The logic was sound: if Vitamin E stops oxidation, and oxidation causes heart disease, then Vitamin E should stop heart disease.
However, large clinical trials have mostly failed to prove this. The US Preventive Services Task Force (USPSTF) reviewed the evidence in 2022 and recommended against using Vitamin E supplements for the prevention of cardiovascular disease or cancer, concluding there is no net benefit.
Similarly, the massive GISSI-Prevenzione trial followed over 11,000 heart attack survivors. While Omega-3 fatty acids reduced the risk of death, Vitamin E supplementation provided no benefit.
4. Brain Health and Alzheimer’s
The brain is rich in fats, making it a prime target for Vitamin E protection. A 2019 review noted that while people with Alzheimer’s often have lower Vitamin E levels, supplementation trials have been inconsistent. Some data suggests high-dose Vitamin E might slow functional decline in existing Alzheimer’s disease, but a 2015 study clarified that it provided no cognitive benefit for healthy older adults or those with mild cognitive impairment.
The “Goldilocks” Problem: Why Supplements Fail
Why does eating Vitamin E-rich foods (like almonds and spinach) seem to help, while pills often fail?
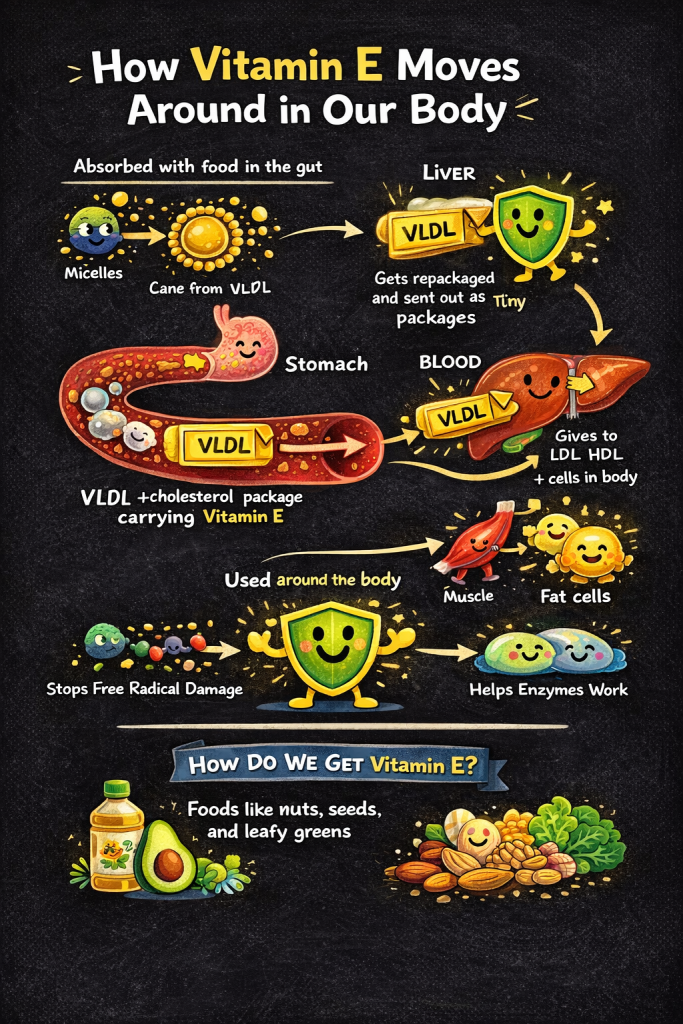
1. The Liver’s Gatekeeper
Your liver is incredibly strict about Vitamin E. According to research on Vitamin E metabolism, a protein called alpha-tocopherol transfer protein (alpha-TTP) regulates how much Vitamin E gets into your blood. If you take a massive dose, the liver simply breaks down and excretes the excess. This natural ceiling limits how much you can “supercharge” your blood levels.
2. Drug Interactions
High doses of Vitamin E are not biologically inert. Research in Vitamins and Hormones suggests that high levels of Vitamin E can upregulate enzymes in the liver (specifically CYP3A) that metabolize drugs. This means taking a high-dose Vitamin E supplement could potentially cause your body to process other medications too quickly, making them less effective.
3. The Vitamin K Connection
There is also evidence that high-dose Vitamin E can interfere with Vitamin K, which is necessary for blood clotting. A 2008 review noted that while Vitamin E might reduce the risk of sudden death from clots (a benefit), it can also increase the risk of bleeding events (a harm). This delicate balance makes unsupervised high-dose supplementation risky.
Who Benefits Or Needs Caution
Who Likely Benefits
- Patients with NASH: Under medical supervision, Vitamin E is one of the few interventions shown to help non-alcoholic fatty liver disease.
- People with Malabsorption Issues: Conditions like Cystic Fibrosis, Crohn’s disease, or those who have had gastric bypass often cannot absorb fat-soluble vitamins and require supplementation.
- The 90%: A 2014 review estimated that over 90% of Americans do not consume the estimated average requirement of dietary Vitamin E. The solution here is likely dietary improvement, not mega-dosing.
Who Should Be Careful
- People on Blood Thinners: Due to the interaction with Vitamin K and clotting, Vitamin E can increase bleeding risk.
- Those taking other medications: Because Vitamin E can alter liver enzymes, it may interact with statins, chemotherapy, or other drugs.
Practical Guidance: Food First
Because the body regulates Vitamin E so tightly, and because the different forms found in food (like gamma-tocopherol) may have benefits that synthetic alpha-tocopherol supplements lack, getting this nutrient from food is the safest strategy.
Top Sources:
- Sunflower seeds
- Almonds
- Hazelnuts
- Spinach and Swiss chard
- Avocado
- Olive oil
The Bottom Line
Vitamin E is a critical nutrient that protects your cell membranes from breaking down. However, the scientific evidence does not support taking high-dose supplements for general disease prevention in healthy people. The body has a complex system for regulating Vitamin E levels, suggesting that “more” is not necessarily better.
While specific conditions like fatty liver disease (NASH) respond well to Vitamin E therapy, for most people, the goal should be meeting the daily requirement through nuts, seeds, and leafy greens rather than pills.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Fatty Liver (NASH) | Vitamin E (800 IU) significantly improved liver health in non-diabetic NASH patients. | PMID 20427778 |
| Heart Disease | Vitamin E supplements did not reduce heart attacks or death in myocardial infarction survivors. | PMID 10465168 |
| General Prevention | USPSTF recommends against Vitamin E supplements for preventing cardiovascular disease or cancer. | PMID 35727271 |
| Dietary Intake | >90% of Americans do not consume enough dietary Vitamin E. | PMID 25469382 |
| Alzheimer’s | Vitamin E did not improve cognitive function in healthy older adults or those with mild impairment. | PMID 26618765 |
| PUFA Interaction | Vitamin E requirements increase as intake of polyunsaturated fats increases. | PMID 26291567 |
Last updated: February 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply