You sleep for eight full hours, yet you wake up feeling like you barely rested at all. Throughout the day, you struggle to concentrate. Your partner mentions that you snore loudly or seem to stop breathing during the night. If this sounds familiar, you might be dealing with obstructive sleep apnea.
Obstructive sleep apnea (ob-STRUK-tiv sleep AP-nee-uh) is a condition where the muscles in the back of your throat relax too much during sleep. This causes your airway to narrow or close completely, cutting off your oxygen supply. Your brain senses the danger and briefly wakes you up to reopen the airway. This cycle can happen dozens of times an hour, preventing you from getting deep, restorative sleep.
For decades, the standard answer to this problem has been a single device. However, recent scientific reviews show that treatment is moving toward a highly personalized approach. Researchers now understand that sleep apnea is not just a simple plumbing problem. It involves complex interactions between your anatomy, your nervous system, and your metabolism.
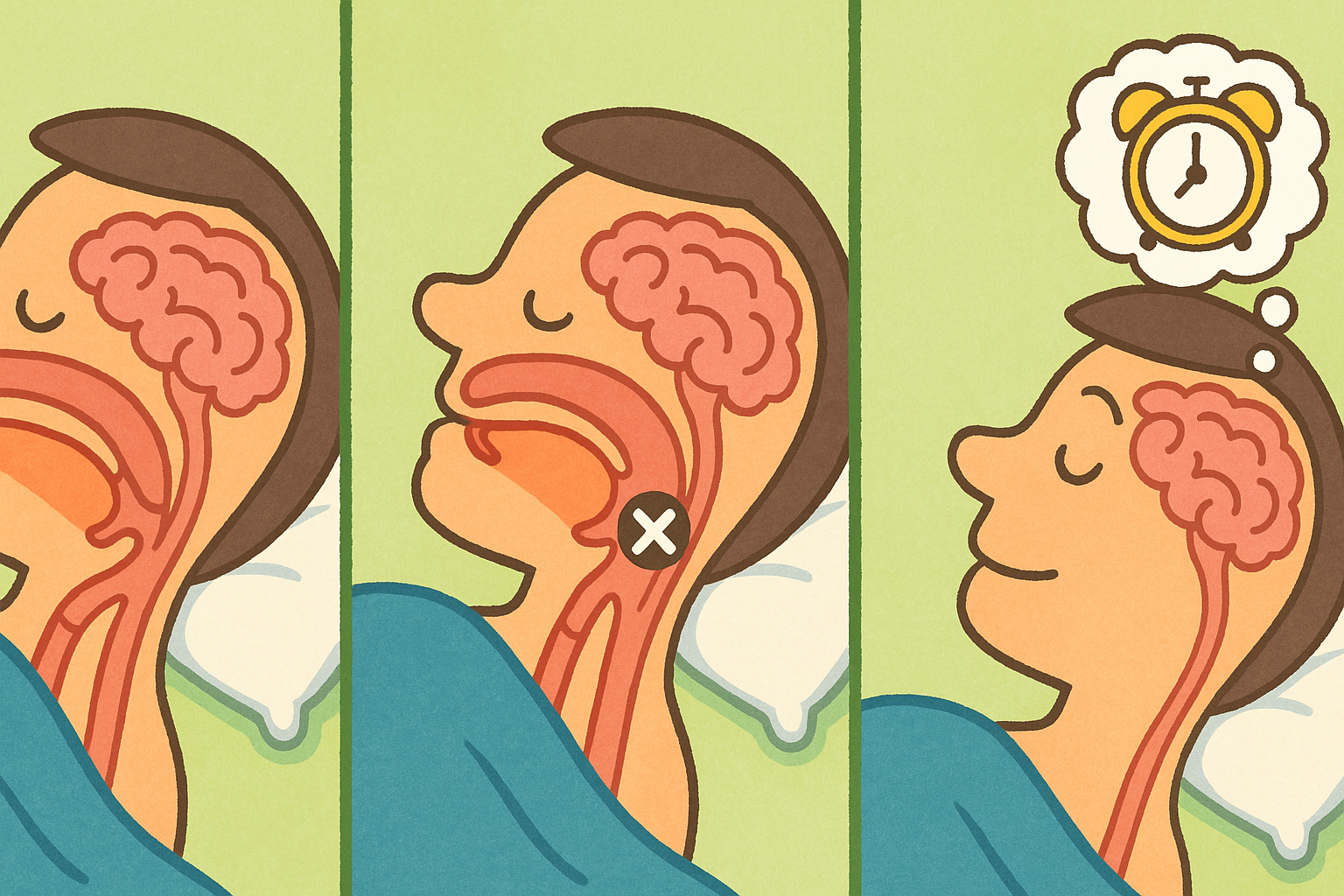
This article explores what the latest peer-reviewed research says about treating obstructive sleep apnea, how different therapies work, and why the future of treatment is highly customized.
How This Might Work: The Mechanics of Sleep Apnea
To understand how treatments work, it helps to understand why the airway collapses in the first place. For a long time, doctors focused mostly on physical blockages, like large tonsils or excess weight around the neck.
However, a 2016 review in the Annals of the American Thoracic Society highlights that obstructive sleep apnea is actually driven by four distinct physical traits:
1. Anatomy: Some people naturally have a narrower airway or a physical structure that collapses easily under pressure.
2. Muscle Control: The muscles that hold the airway open, especially the tongue, may not respond quickly enough when oxygen levels drop.
3. Arousal threshold (uh-ROW-zul THRESH-hold): This refers to how easily your brain wakes you up. If your threshold is too low, you wake up before your airway muscles have a chance to fix the problem themselves.
4. Loop gain (loop gayn): This describes how sensitive your brain is to changes in carbon dioxide. A highly sensitive brain will cause you to breathe too heavily, which can create a vacuum effect that pulls the airway shut again.
Doctors measure the severity of the condition using the Apnea-hypopnea index (AP-nee-uh hy-POP-nee-uh IN-dex), or AHI. This number represents how many times your breathing stops or becomes dangerously shallow per hour of sleep.
While the AHI is helpful, a 2021 study in Lung points out that this single number does not tell the whole story. Two people with the exact same AHI might need completely different treatments based on which of the four physical traits is causing their airway to collapse.
What the Research Shows: The Gold Standard Treatment
The most common and effective treatment for obstructive sleep apnea is a Continuous Positive Airway Pressure machine, commonly known as CPAP.
A CPAP machine works by gently blowing pressurized air through a mask into your nose or mouth. This constant flow of air acts like an invisible splint, keeping the walls of your throat from caving in while you sleep.
The Benefits of CPAP
When used consistently, CPAP therapy has profound effects on the entire body.
- Heart Health: A 2024 review in Clinica e investigacion en arteriosclerosis found that sleep apnea triggers a stress response in the body, leading to high blood pressure and blood vessel damage. CPAP therapy helps lower blood pressure, especially in people who have hypertension that does not respond well to medications.
- Brain Health and Memory: Sleep apnea deprives the brain of oxygen and causes neuroinflammation. A 2025 review in Sleep Medicine Reviews explains that CPAP treatment can provide remarkable relief from memory impairment, helping people regain focus and cognitive function.
- Metabolic Health: Poor sleep disrupts how the body handles sugar and insulin. Treating sleep apnea can improve these metabolic markers.
Related: Continuous Glucose Monitors: What the Latest Science Actually Says
The Adherence Problem
Despite its benefits, CPAP therapy has a major limitation. People struggle to use it.
According to a 2020 review in Sleep Medicine Clinics, about 30 to 40 percent of patients do not wear their CPAP consistently. Common complaints include discomfort from the mask, dry mouth, feeling claustrophobic, or being bothered by the pressure of the air.
Research shows that to get the cardiovascular and brain benefits, a patient needs to wear the CPAP for at least four hours a night. Because adherence is such a challenge, scientists have heavily researched alternative treatments.
How This Compares To Alternatives
For people who cannot tolerate a CPAP machine, or for those with milder forms of sleep apnea, several other evidence-based treatments exist.
Oral Appliances
An oral appliance looks similar to a sports mouthguard. It is custom-fitted by a dentist and works by pulling the lower jaw slightly forward. This physical shift moves the base of the tongue away from the back of the throat, creating more space for air to flow.
A 2009 clinical guideline from the Journal of Clinical Sleep Medicine confirms that oral appliances are an effective alternative for people with mild to moderate sleep apnea. While they are generally less effective than CPAP at completely eliminating breathing pauses, many patients find them much easier to wear all night.
Myofunctional Therapy (Throat Exercises)
Just as you can lift weights to strengthen your arms, you can perform targeted exercises to strengthen your tongue and throat muscles. This is known as myofunctional therapy (my-oh-FUNK-shun-al THAIR-uh-pee).

A comprehensive 2015 meta-analysis in Sleep reviewed data from 120 adults and 25 children who practiced these exercises. The results were notable. In adults, myofunctional therapy decreased the apnea-hypopnea index by roughly 50 percent. It also improved blood oxygen levels and reduced snoring. In children, the therapy decreased breathing pauses by 62 percent.
While throat exercises rarely cure severe sleep apnea on their own, the research shows they are an excellent companion treatment that can make a noticeable difference.
Positional Therapy
For some people, sleep apnea only happens, or gets much worse, when they sleep flat on their backs. Gravity pulls the tongue and soft palate downward, blocking the airway. This is called positional sleep apnea.
A 2024 review in the Otolaryngologic Clinics of North America examined positional therapy devices. In the past, doctors told patients to sew a tennis ball into the back of their pajama shirt to prevent back-sleeping. Today, small electronic devices worn on the chest or neck vibrate gently when the sleeper rolls onto their back, prompting them to turn over without fully waking up. The research notes that these new devices have high compliance rates and offer substantial relief for people whose apnea is tied to their sleep position.
Weight Management
There is a strong connection between excess body weight and sleep apnea. Fat deposits around the upper airway can narrow the breathing passage, and extra weight on the chest can reduce lung volume.
A 2024 review in Sleep Medicine Reviews looked at the impact of weight loss on the condition. The researchers found that significant weight loss, whether through lifestyle changes, bariatric surgery, or new anti-obesity medications, often leads to a major improvement in sleep apnea symptoms.
However, the researchers caution that sleep apnea is not exclusively a weight issue. Many people with normal body weights have severe sleep apnea due to their facial structure or muscle control. Therefore, weight loss is a helpful tool, but it is not a guaranteed cure for everyone.
Related: GLP-1 Weight Loss Drugs: What Real-World Results Actually Show
Who Benefits Or Needs Caution: The REM Sleep Difference
When evaluating treatment options, doctors are learning that the stage of sleep matters.
Sleep is divided into cycles, including rapid eye movement (REM) sleep and non-REM sleep. During REM sleep, the brain actively paralyzes most of the body’s skeletal muscles to prevent you from acting out your dreams. Unfortunately, this paralysis also affects the muscles that keep the airway open.
A 2024 study in the European Respiratory Review focused on a specific subtype called REM-related obstructive sleep apnea. The researchers found several unique patterns:
- It affects women more often: REM sleep apnea is significantly more common in women than in men.
- The events are longer: Because the muscles are deeply relaxed, breathing pauses during REM sleep tend to last longer and cause more severe drops in oxygen.
- Timing matters for CPAP: REM sleep occurs mostly in the second half of the night. If a patient takes their CPAP mask off after four hours, they are leaving themselves completely unprotected during the exact time their airway is most vulnerable.
People with REM-related sleep apnea may have a low overall AHI score, making their condition look mild on paper. However, they often experience the same level of daytime exhaustion and cardiovascular risk as those with severe apnea.
Where The Science Is Going: Implants and Artificial Intelligence
For patients who cannot tolerate CPAP and do not get relief from oral appliances, the scientific focus is shifting toward technology and surgical implants.
Hypoglossal Nerve Stimulation
One of the most studied surgical options is the hypoglossal nerve stimulator. This involves implanting a small device, similar to a pacemaker, under the skin of the chest.
A 2024 review in the Otolaryngologic Clinics of North America explains how this works. The device monitors your breathing patterns. Right before you take a breath, it sends a mild electrical pulse to the hypoglossal nerve, which controls the tongue. This pulse pushes the tongue slightly forward, keeping the airway clear. The therapy is highly effective for specific patients, but it requires careful screening to ensure the patient’s airway collapses in a way that the device can actually fix.
Artificial Intelligence
Artificial intelligence is beginning to change how doctors choose treatments. A 2023 review in the Journal of Otolaryngology explored how machine learning is being used in sleep medicine.
Instead of trial and error, doctors can now use AI to analyze a patient’s sleep study data, audio recordings of their snoring, and their physical traits. The AI can predict with high accuracy whether a patient will actually use a CPAP machine, whether an oral appliance will work for their specific jaw shape, or if they are a good candidate for surgery.
Common Questions About Obstructive Sleep Apnea
Does weight loss cure sleep apnea?
Weight loss can significantly reduce the severity of sleep apnea, and in some cases of mild apnea, it may resolve the issue. However, because airway anatomy and brain reflexes also play a role, many people still need treatment even after reaching a moderate weight.
Can medications treat sleep apnea?
Currently, there is no pill that cures sleep apnea. A 2021 review in Sleep Medicine Reviews notes that while some medications are prescribed to help patients stay awake during the day, they only mask the symptom of exhaustion. They do not stop the airway from collapsing at night.
How long do I need to wear a CPAP each night?
Research shows you need to wear it for a minimum of four hours to see cardiovascular benefits. However, because the most severe breathing pauses often happen during REM sleep in the early morning hours, wearing it for the entire duration of your sleep is highly recommended.
The Bottom Line
Obstructive sleep apnea is a complex condition that impacts the heart, brain, and metabolism.
- CPAP remains the most effective and widely researched treatment, offering proven benefits for blood pressure, memory, and daytime energy.
- Because CPAP can be difficult to wear, alternatives like oral appliances, throat exercises, and positional therapy devices offer solid, evidence-based options for many people.
- The future of sleep medicine is moving away from a single solution. By understanding exactly why your airway collapses, doctors can use targeted therapies, implants, and AI predictions to find the treatment that works best for your specific biology.
If you suspect you have sleep apnea, a formal sleep study is the only way to accurately diagnose the condition and determine which physical traits are causing the obstruction.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Personalized Treatment | OSA is driven by four physical traits: anatomy, muscle control, arousal threshold, and loop gain. | PMID 26569377 |
| Memory and Brain Health | CPAP treatment provides remarkable relief from memory impairment caused by sleep apnea. | PMID 40286536 |
| Heart Health | CPAP reduces blood pressure and cardiovascular risk, but only if used for at least 4 hours a night. | PMID 38413245 |
| Throat Exercises | Myofunctional therapy decreased the apnea-hypopnea index by roughly 50% in adults and 62% in children. | PMID 25348130 |
| REM Sleep Apnea | Apneas during REM sleep are longer, more severe, and more common in women. | PMID 38355150 |
| Artificial Intelligence | AI can accurately predict whether a patient will respond well to oral appliances or surgery. | PMID 36747273 |
| Nerve Stimulation | Hypoglossal nerve stimulators are an effective alternative for patients who cannot tolerate CPAP. | PMID 38521724 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply