Managing your cholesterol can often feel like navigating a maze of conflicting advice. One day you are told to avoid eggs, the next day you are told to drink specialized teas, and all the while, your doctor might be recommending prescription medication.
When it comes to cardiovascular health, understanding your cholesterol is critical. A 2022 study in the International Journal of Preventive Medicine analyzing predictive models for heart attacks found that alongside blood pressure and smoking, cholesterol levels remain one of the most significant predictors of a future myocardial infarction (my-oh-KAR-dee-ul in-FARK-shun), the medical term for a heart attack.
But what actually works to bring those numbers down? Does drinking herbal tea make a real difference, or are prescription medications the only reliable route? By looking at recent clinical trials, meta-analyses, and behavioral studies, we can separate the proven strategies from the wishful thinking.
Understanding the Cholesterol Highway
Before diving into the treatments, it helps to understand how cholesterol works. You can think of your bloodstream as a highway system. Cholesterol is a waxy, fat-like substance that your body needs to build cells and make hormones. Because it is fat-based, it cannot travel through your watery blood on its own. It needs a vehicle.
These vehicles are called lipoproteins:
- LDL (Low-Density Lipoprotein): Often called “bad” cholesterol. Think of LDL as delivery trucks that are prone to crashing. When there are too many of them, they crash into the walls of your arteries, causing traffic jams known as plaque.
- HDL (High-Density Lipoprotein): Often called “good” cholesterol. Think of HDL as the tow trucks or garbage trucks. They travel through the bloodstream, picking up excess cholesterol and taking it back to the liver to be processed and removed.
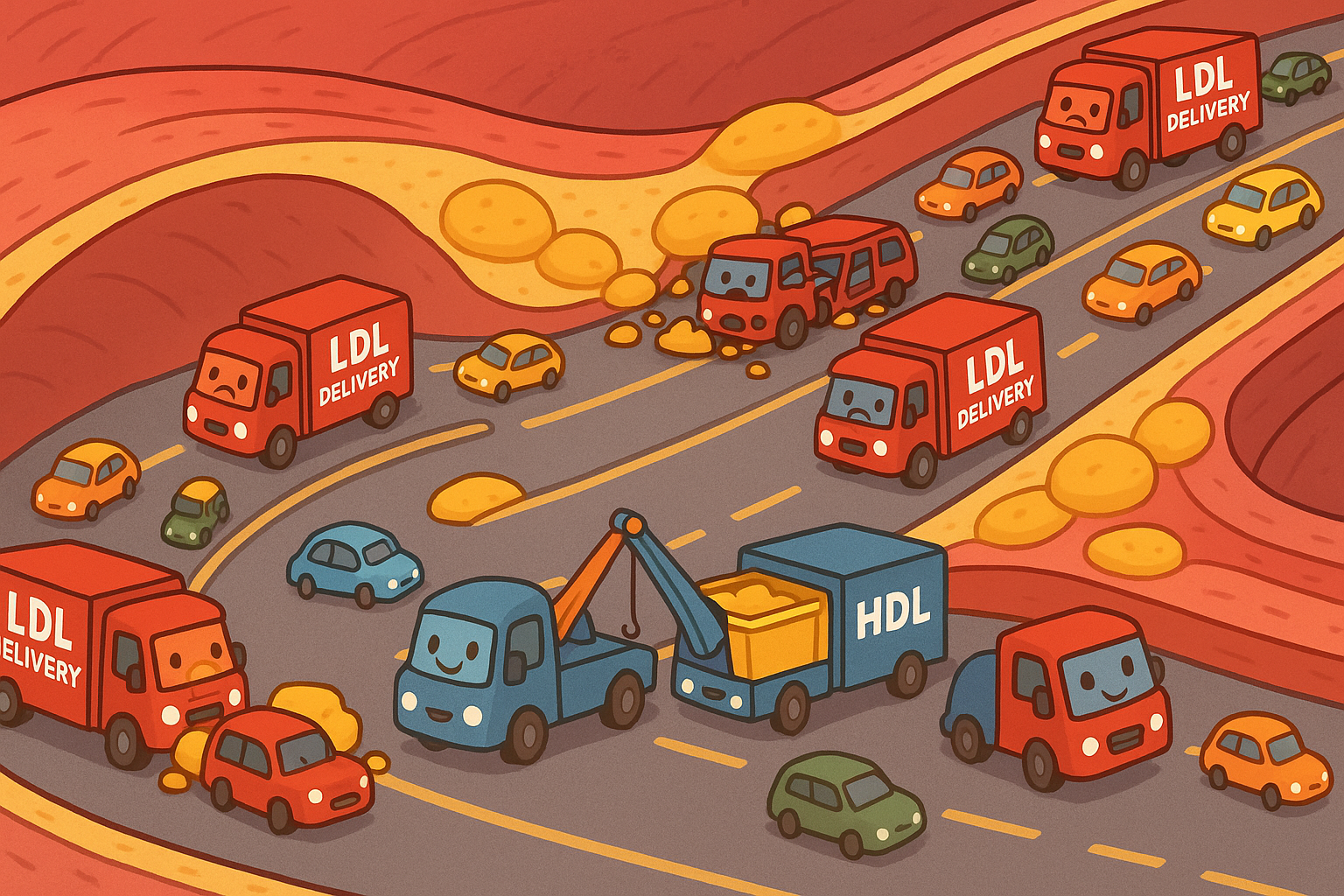
When plaque builds up, it causes atherosclerosis (ath-er-o-skluh-RO-sis), a hardening and narrowing of the arteries that restricts blood flow. The goal of cholesterol management is to reduce the number of LDL delivery trucks and keep the highway clear. Related: Why ApoB Might Be the Most Accurate Heart Health Test You Have Never Had
What the Research Shows: The Medical Approach
When lifestyle changes are not enough to lower cholesterol, doctors turn to medication. The scientific consensus on these treatments is robust, though how they are prescribed is evolving.
Optimizing Statin Therapy
Statins are the most common and effective class of drugs used to lower LDL cholesterol. They work by blocking an enzyme your liver needs to make cholesterol.
A 2024 review in Mayo Clinic Proceedings outlined the top tips for using statins in clinical practice. The researchers emphasized that while statins are highly effective, many patients stop taking them due to perceived side effects or complex dosing schedules. The research highlights the importance of matching the statin intensity to the patient’s specific cardiovascular risk profile.
For patients who experience muscle aches, a common complaint, the guidelines suggest working closely with a doctor to adjust the dose, switch to a different type of statin, or evaluate for drug interactions rather than abandoning the medication entirely. Related: Understanding Your Coronary Calcium Score: What the Numbers Actually Mean
The Rise of the “Polypill”
One of the biggest hurdles in managing cardiovascular health is “pill fatigue.” Taking a separate pill for cholesterol, blood pressure, and blood thinning can be exhausting. Enter the polypill (PAH-lee-pill), a single capsule that combines several cardiovascular drugs into one dose.

A 2023 review in Current Problems in Cardiology noted that polypills hold massive potential to increase patient compliance, reduce costs, and provide psychological relief for patients managing multiple conditions.
But does combining these drugs dilute their effectiveness? A major clinical trial known as the Second Indian Polycap Study (TIPS-2), published in Circulation: Cardiovascular Quality and Outcomes, tested this exact question. Researchers studied 518 individuals at high risk for cardiovascular disease. They compared a low-dose polypill against a full-dose polypill (which contained higher doses of blood pressure medications, aspirin, and 20 mg of the statin simvastatin).
The results were clear. The full-dose polypill reduced LDL cholesterol by an additional 6.6 mg/dL compared to the low dose. It also provided superior blood pressure reduction. Importantly, the full-dose version was tolerated just as well as the low-dose version, with similar dropout rates between the two groups. This suggests that combining full-strength medications into a single pill is both safe and highly effective for managing cholesterol and overall heart risk.
Do Natural Teas and Herbs Actually Lower Cholesterol?
Many people prefer to start with natural remedies before turning to prescription medications. The scientific literature shows that certain plants do have a measurable impact on lipid levels, though the effects are generally more modest than pharmaceutical options.
Green Tea and Black Seed
A massive 2020 meta-analysis in Phytotherapy Research reviewed 279 clinical trials to evaluate the effect of herbal medicines on obesity and metabolic syndrome.
The researchers found strong evidence supporting green tea extract. Across multiple trials, consuming green tea resulted in significant improvements in total cholesterol, LDL cholesterol, and body weight. The active compounds in green tea, known as catechins, appear to inhibit fat absorption and increase energy expenditure.
The same review found that Nigella sativa, commonly known as black seed, resulted in a significant improvement in triglyceride levels. Triglycerides are another type of fat in the blood that, when elevated, increase the risk of heart disease.
Hibiscus (Sour Tea)
Hibiscus tea, known in some regions as sour tea or karkade, is a bright red beverage popular worldwide. A 2020 systematic review in Food Research International analyzed eight randomized clinical trials involving nearly 500 subjects to see if hibiscus actually improves metabolic health.
The pooled data showed that hibiscus consumption significantly reduced fasting blood glucose and LDL cholesterol. The researchers attribute this to the high concentration of anthocyanins and polyphenols in the plant, which act as antioxidants and may help inhibit the enzymes involved in fat synthesis. However, the study noted that hibiscus did not have a statistically significant impact on raising HDL (good) cholesterol or lowering total triglycerides.
How Behavioral Science Impacts Your Success
Knowing what to do is only half the battle. Actually doing it is where most people struggle. Interestingly, the way you set your lifestyle goals can dictate how successful you are at lowering your cholesterol and blood pressure.
A 2018 randomized controlled trial in the American Journal of Preventive Medicine looked at the effectiveness of web-based lifestyle counseling. Researchers divided 128 patients into three groups:
1. Control Group: Received basic weekly health newsletters.
2. User-Driven Group: Received weekly emails allowing them to choose their own health goals and interventions.
3. Expert-Driven Group: Received a prescribed, specific weekly exercise and diet plan (e.g., “increase your steps by 1,000 this week”).
After four months, the expert-driven group saw the most dramatic improvements. They had significantly greater reductions in systolic blood pressure, total cholesterol, and their overall 10-year cardiovascular risk compared to the control group. They also increased their daily step count and fruit intake more than the user-driven group.
This suggests that when trying to change your lifestyle to lower cholesterol, removing the burden of choice helps. Having a clear, expert-prescribed plan is often more effective than trying to design a custom routine yourself.
Who Needs Extra Caution
While lifestyle and standard medications work for most, certain populations face unique challenges with cholesterol management.
People taking psychiatric medications: A 2009 review in Acta Psychiatrica Scandinavica highlighted that patients taking atypical antipsychotics are at a much higher risk for cardiometabolic issues, including severe dyslipidemia (dis-lip-ih-DEE-mee-uh), which is an abnormal amount of lipids in the blood.
The research indicates that some of these medications can cause insulin resistance and high triglycerides even in the absence of weight gain. Patients on these medications require much closer monitoring of their cholesterol levels, as their risk is driven by the medication’s effect on their biology, not just their lifestyle choices.
Where the Science is Heading: Nanotechnology
Scientists are constantly looking for ways to make natural compounds more effective. Resveratrol is a well-known compound found in the skin of red grapes that has shown cardiovascular benefits. However, the human body struggles to absorb it efficiently.
A 2025 study in the Journal of Liposome Research tested a novel solution in an animal model. Researchers packed resveratrol into nanoliposomes (NAN-oh-LIP-oh-sohms), which are microscopic fat bubbles designed to protect the compound and deliver it directly to cells.
When given to rats on a high-fat diet, the nanoliposome-delivered resveratrol significantly reduced total cholesterol, LDL, and triglycerides while increasing HDL. It also reduced liver damage caused by the high-fat diet. While this is an animal study and cannot yet be applied to humans, it represents an exciting frontier where natural compounds are supercharged by modern drug delivery technology.
Practical Guidance
Based on the synthesis of these studies, here is how you can practically apply the science to your daily life:
- Follow a Prescribed Plan: If you are trying to lower your cholesterol through diet and exercise, do not guess. Find a structured, expert-designed plan. Research shows that being told exactly what to do (expert-driven) leads to better cholesterol reductions than trying to design your own routine.
- Incorporate Evidence-Based Teas: Swapping sugary drinks for green tea or hibiscus tea is a science-backed way to moderately lower LDL cholesterol and blood sugar. Just remember that these are supplements to, not replacements for, medical care.
- Talk to Your Doctor About Polypills: If you struggle to remember to take your cholesterol and blood pressure medications, ask your doctor if a combination pill is right for you. They are proven to be highly effective and can greatly simplify your morning routine.
- Communicate About Side Effects: If a statin gives you muscle aches, do not just stop taking it. Work with your doctor to adjust the dose or switch brands. The cardiovascular protection they offer is too significant to abandon without a conversation.
The Bottom Line
Cholesterol management is not an either-or scenario between natural remedies and modern medicine. The research shows that lifestyle interventions, like drinking green tea or following a structured exercise program, can meaningfully improve your lipid profile. However, for those at high risk, medications like statins and combination polypills remain the most powerful, proven tools for clearing the “cholesterol highway” and preventing heart attacks.
What remains uncertain is exactly how future technologies, like nanoliposome delivery for natural compounds, will translate from animal models to human treatments. For now, the best approach is a collaborative one: use evidence-based lifestyle habits to support your body, and rely on well-managed medical therapies to do the heavy lifting when needed.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Statins in Clinical Practice | Outlines guidelines for optimizing statin use, managing side effects, and assessing cardiovascular risk accurately. | PMID 39631991 |
| Polypill Dosing (TIPS-2) | A full-dose combination pill lowered LDL by an extra 6.6 mg/dL compared to a low-dose pill, with similar tolerability. | PMID 22787067 |
| Herbal Medicines & Obesity | Meta-analysis of 279 trials found green tea significantly reduces LDL and total cholesterol, while black seed lowers triglycerides. | PMID 31793087 |
| Hibiscus Tea Effects | Meta-analysis showed Hibiscus sabdariffa significantly lowers LDL cholesterol and fasting blood glucose. | PMID 32156406 |
| Web-Based Counseling | Expert-driven digital health plans resulted in better cholesterol and blood pressure reductions than user-driven plans. | PMID 29456025 |
| Antipsychotics & Lipid Risk | Atypical antipsychotics can cause severe dyslipidemia and insulin resistance, sometimes independent of weight gain. | PMID 19178394 |
Last updated: May 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply