The Rise of Childhood Allergies and Asthma
If you walk into any modern elementary school classroom, you will likely see a familiar sight: asthma inhalers stored in the nurse’s office and allergy warning signs posted on the wall. Over the past 50 years, the rates of childhood asthma and allergic diseases have risen dramatically around the world.
This rapid increase has left many parents and researchers asking a core question: Why do some children develop these conditions while others do not?
The short answer is that there is no single cause. A 2025 review in Mucosal Immunology and decades of global research show that childhood allergies and asthma result from a complex interaction between a child’s genetics, their early environment, their diet, and the trillions of bacteria living in and on their bodies.
While we cannot change a child’s genes, scientists are uncovering how early life exposures train the immune system either to tolerate harmless substances or to mount a severe allergic defense.
The Atopic March: How Allergies Progress
To understand childhood allergies, we first need to understand how they typically develop. Pediatricians often observe that allergic conditions do not appear randomly. Instead, they tend to follow a specific timeline.

This progression is known as the Atopic march (uh-TOP-ik march), which is the tendency for allergic diseases to appear in a specific sequence starting in infancy. According to a 2020 review in Frontiers in Immunology, the march usually begins with skin issues, progresses to food allergies, and eventually leads to respiratory issues like asthma and allergic rhinitis (hay fever).
The Role of the Skin Barrier
The skin is the body’s first line of defense. In many children, the atopic march starts with eczema (atopic dermatitis) in the first few months of life.
Researchers have discovered that a protein called Filaggrin (fill-AG-rin) plays a crucial role in keeping the skin barrier strong and hydrated. Some children have genetic variations that reduce their filaggrin levels, leading to dry, cracked skin.
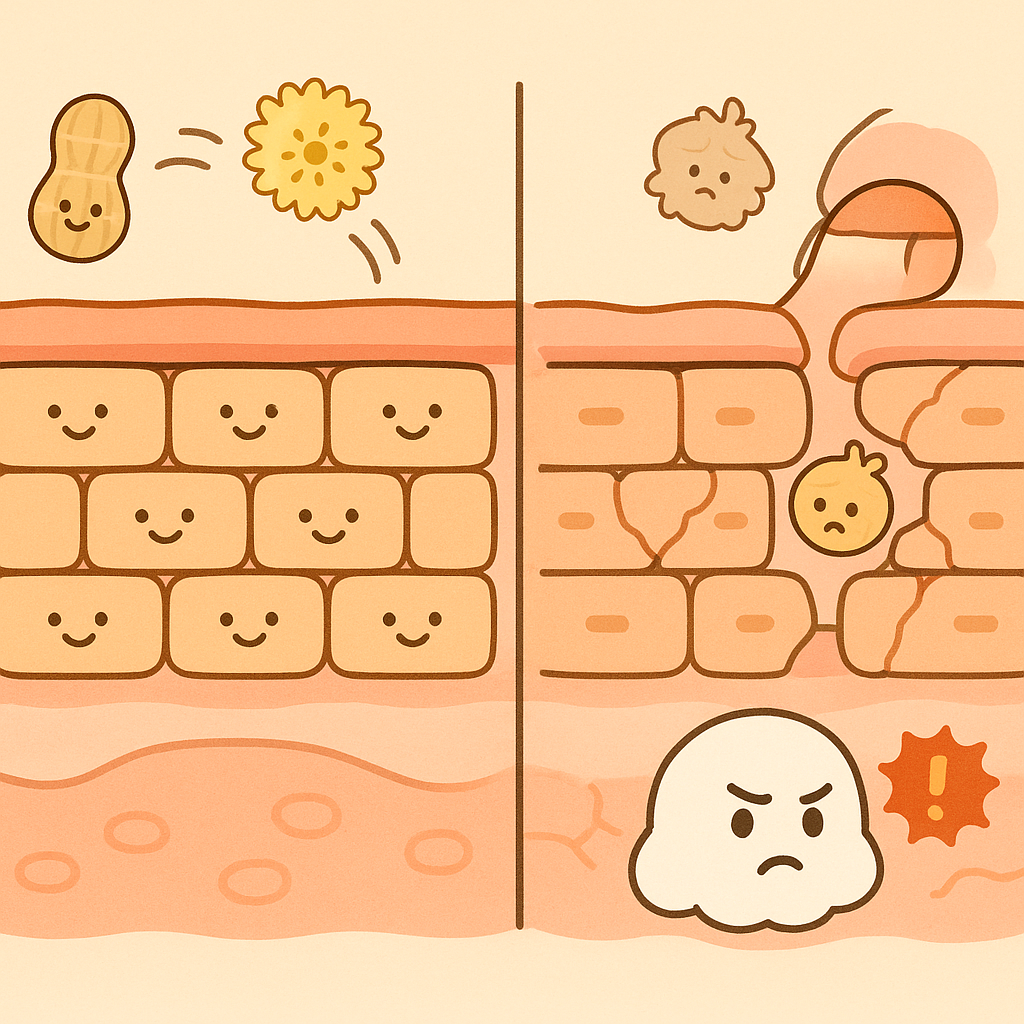
When the skin barrier is damaged, environmental allergens like peanut dust, pet dander, or pollen can bypass the surface and enter the body. The immune system, encountering these substances through broken skin rather than through the digestive tract, misidentifies them as dangerous invaders. This process, called transcutaneous sensitization, can trigger the immune system to produce allergy antibodies, setting the stage for future food allergies and asthma.
Related: How Your Skin Barrier Actually Works: What the Science Shows
What the Research Shows: Genetics and Epigenetics
A child’s risk of developing asthma and allergies is heavily influenced by their family history. A 2023 study in the Journal of Assisted Reproduction and Genetics confirmed that having biological parents with allergies or asthma significantly increases a child’s odds of developing similar conditions.
Scientists have identified numerous genetic markers associated with asthma. For example, a 2021 review in the International Journal of Molecular Sciences highlights a specific genetic region known as 17q21, which is strongly linked to childhood-onset asthma.
However, genetics alone cannot explain the recent spike in allergy rates, because human genes do not change that quickly. Instead, scientists are looking at Epigenetics (ep-ih-juh-NET-iks), which refers to changes in how genes are turned on or off without altering the underlying DNA code. Environmental factors like air pollution, diet, and tobacco smoke can cause epigenetic changes that increase inflammation and allergy risk.
The Microbiome and The “Farm Effect”
One of the most heavily researched areas in allergy prevention is the hygiene hypothesis, which has recently evolved into the biodiversity hypothesis. This theory suggests that modern, highly sanitized environments lack the diverse microbes needed to properly train a child’s immune system.
The Protective Power of Farms
A 2022 review in Pediatric Allergy and Immunology explored a phenomenon known as the “Farm Effect.” Multiple worldwide studies have shown that children who grow up on traditional dairy farms have significantly lower rates of asthma and allergies compared to children in urban environments.
Researchers attribute this protection to a high exposure to diverse environmental microbes found in animal sheds, hay, and unprocessed farm milk. These microbes contain compounds like endotoxins that stimulate the innate immune system. Instead of causing illness, this early, low-grade exposure teaches the immune system to remain calm and produces regulatory T-cells, which act as the immune system’s peacekeepers.

The Infant Gut Microbiome
The bacteria living in a baby’s digestive tract, known as the Microbiome (my-kroh-BY-ohm), play a massive role in immune development.
A 2016 study in Nature Medicine analyzed the stool of infants and categorized their gut microbiomes into three distinct states. Infants in the third state (NGM3) had lower levels of helpful bacteria like Bifidobacterium and higher levels of certain fungi. These infants had a significantly higher risk of developing multiple allergies by age two and asthma by age four.
Furthermore, a 2025 study in The Journal of Allergy and Clinical Immunology found that specific microbes in the infant gut, such as Blautia obeum, are associated with a reduced risk of food and inhalant allergies. The researchers noted that a child’s genetics interact directly with their environment to shape this microbial community.
Related: Probiotics and Gut Health: What the Science Actually Shows
How Diet Influences Allergy Risk
What a mother eats during pregnancy, and what a child eats in their early years, can impact immune programming.
Maternal Diet During Pregnancy
A 2020 systematic review by the European Academy of Allergy and Clinical Immunology analyzed how a mother’s diet during pregnancy affects her child’s allergy risk. The strongest evidence pointed to Vitamin D. The meta-analysis showed that maternal prenatal Vitamin D supplementation was associated with a reduced risk of wheezing and asthma in offspring.
Omega-3 fatty acids (found in fish) showed a trend toward protecting against asthma and allergic rhinitis, though the results were not always statistically significant. The review found no consistent evidence that maternal diet alone could prevent eczema or food allergies.
Additionally, a 2022 systematic review in Nutrients looked at whether pregnant women taking probiotics could reduce their child’s allergy risk. The results were mixed, but some studies suggested that taking a combination of lactobacilli and bifidobacteria during pregnancy and shortly after birth might reduce the risk of infant eczema, particularly in families with a strong history of allergies.
Human Milk and Childhood Diet
Breast milk provides essential nutrients and beneficial bacteria to infants. A 2024 study in Cell Host & Microbe found that the network of microbes in human milk is associated with a child’s future risk of asthma and allergies, and this microbial network is actually influenced by the mother’s genetics.
As children grow, their dietary choices continue to impact their immune health. A 2024 report in Pediatric Allergy and Immunology found that high consumption of ultra-processed foods (UPFs), sugar-sweetened beverages, and excessive fructose is associated with an increased risk of asthma, allergic rhinitis, and food allergies.
Conversely, diets high in fiber help gut bacteria produce Short-chain fatty acids (short-chayn fat-ee as-ids), or SCFAs. SCFAs act as fuel for the cells lining the gut and have strong anti-inflammatory effects that circulate throughout the body, helping to protect the lungs against allergic airway inflammation.
Environmental Triggers: Weight, Pollution, and Viruses
Beyond diet and microbes, several other factors can increase the likelihood of asthma symptoms.
Body Mass Index (BMI)
A 2023 systematic review in Clinical and Experimental Allergy examined how childhood weight affects allergy risk. The researchers found two consistent patterns: a rapid increase in BMI during the first two years of life, and a persistently high BMI between ages 6 and 10, were both associated with an increased risk of developing asthma by age 18.
Air Quality and Tobacco Smoke
Exposure to environmental tobacco smoke is a well-documented risk factor for respiratory issues. A 2013 review in the Italian Journal of Pediatrics highlighted that passive smoke exposure impairs lung function and increases the risk of wheezing and asthma. Similarly, a 2022 study of school children in Poland found that visible mold and dampness in the home were associated with higher rates of asthma, though statistical significance varies depending on the specific study population.
Early Viral Infections
Not all asthma starts with allergies. A 2018 review in the Annals of Allergy, Asthma & Immunology notes that severe respiratory viral infections in infancy, particularly from Respiratory Syncytial Virus (RSV) or Rhinovirus (RV), significantly increase the risk of developing asthma later in childhood. These viruses can damage the delicate airway lining, prompting an inflammatory response that makes the lungs hyper-reactive for years to come.
The Link Between Asthma and Severe Allergies
For children who develop food allergies, having asthma is a critical factor to monitor. Anaphylaxis (an-uh-fuh-LAK-sis) is a severe, life-threatening allergic reaction that requires immediate medical treatment with epinephrine.
A 2019 review in Current Opinion in Allergy and Clinical Immunology investigated the relationship between asthma and anaphylaxis. While having asthma does not necessarily mean a child will experience anaphylaxis, poorly controlled asthma is a major risk factor for fatal or near-fatal allergic reactions.
When a child with uncontrolled asthma has an allergic reaction to food or an insect sting, their already-inflamed airways can constrict rapidly, making breathing incredibly difficult. Therefore, keeping a child’s asthma well-controlled with proper medication is one of the most important steps in preventing severe anaphylactic outcomes.
Related: Understanding Food Allergies in Children: What the Latest Science Shows
Who Needs Caution
Based on current research, certain groups of children may need closer monitoring by a pediatrician or allergist:
- Children with severe, early-onset eczema: Because damaged skin can act as an entry point for allergens, managing eczema early is crucial to potentially slow the atopic march.
- Children with a strong family history: Those whose parents have asthma or severe allergies have a higher genetic predisposition.
- Children with food allergies and asthma: These children require strict asthma control to reduce the risk of severe respiratory complications during an accidental allergic reaction.
Common Questions About Childhood Allergies and Asthma
Does having a pet prevent or cause allergies?
The research on pets is mixed. Some studies suggest that early exposure to dogs in the first year of life can increase microbial diversity and slightly lower the risk of allergies. However, if a child is already sensitized and allergic to an animal, keeping the pet in the home will trigger symptoms and worsen asthma.
Does a C-section delivery increase the risk of asthma?
Some research, including a 2016 review on lung barrier immunity, notes an association between Cesarean section deliveries and a slightly higher risk of childhood asthma. This is thought to be because babies born via C-section miss out on swallowing maternal vaginal microbes, which help seed the infant gut microbiome. However, a C-section is often a medically necessary procedure, and many C-section babies never develop asthma.
Will my child outgrow their asthma?
A 2022 study in Allergy tracked asthma and allergy symptoms from childhood to age 34. They found that while some early childhood wheezing is temporary, symptom patterns usually establish themselves during adolescence and stabilize into adulthood. Children with late-onset wheezing in their teen years often had strong links to environmental exposures like active smoking.
The Bottom Line
The development of childhood allergies and asthma is rarely caused by one single event. It is a puzzle involving genetic predisposition, the integrity of the skin barrier, the diversity of the gut microbiome, and early environmental exposures.
While we cannot alter genetics, science suggests that supporting a healthy microbiome through a fiber-rich diet, minimizing exposure to ultra-processed foods and tobacco smoke, and managing early eczema can support immune health. For children who already have asthma and food allergies, maintaining excellent asthma control is the most effective way to prevent severe, life-threatening allergic reactions.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| The Farm Effect | Growing up on traditional farms with exposure to diverse microbes and farm milk protects against asthma and allergies. | PMID 35754122 |
| Infant Microbiome | Infants with specific gut dysbiosis (lower Bifidobacterium, higher fungi) have a higher risk of developing atopy and asthma. | PMID 27618652 |
| Maternal Diet | Prenatal Vitamin D supplementation is associated with a reduced risk of wheeze and asthma in offspring. | PMID 32524677 |
| Childhood Diet | High consumption of ultra-processed foods (UPFs) and sugars is linked to a higher risk of asthma and food allergies. | PMID 39254357 |
| Asthma & Anaphylaxis | Poorly controlled asthma is a significant risk factor for severe and recurrent anaphylactic reactions. | PMID 31261185 |
| Atopic March | Allergic diseases often progress from infant eczema to food allergies, and later to asthma and allergic rhinitis. | PMID 32973790 |
Last updated: May 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply