The Connection Between Your Gut and Your Brain
Have you ever felt “butterflies” in your stomach when you were nervous? That physical sensation is a direct result of the biological connection between your digestive system and your brain. Scientists call this two-way communication network the microbiota-gut-brain axis (my-kro-by-OH-tuh gut brayn AK-sis).
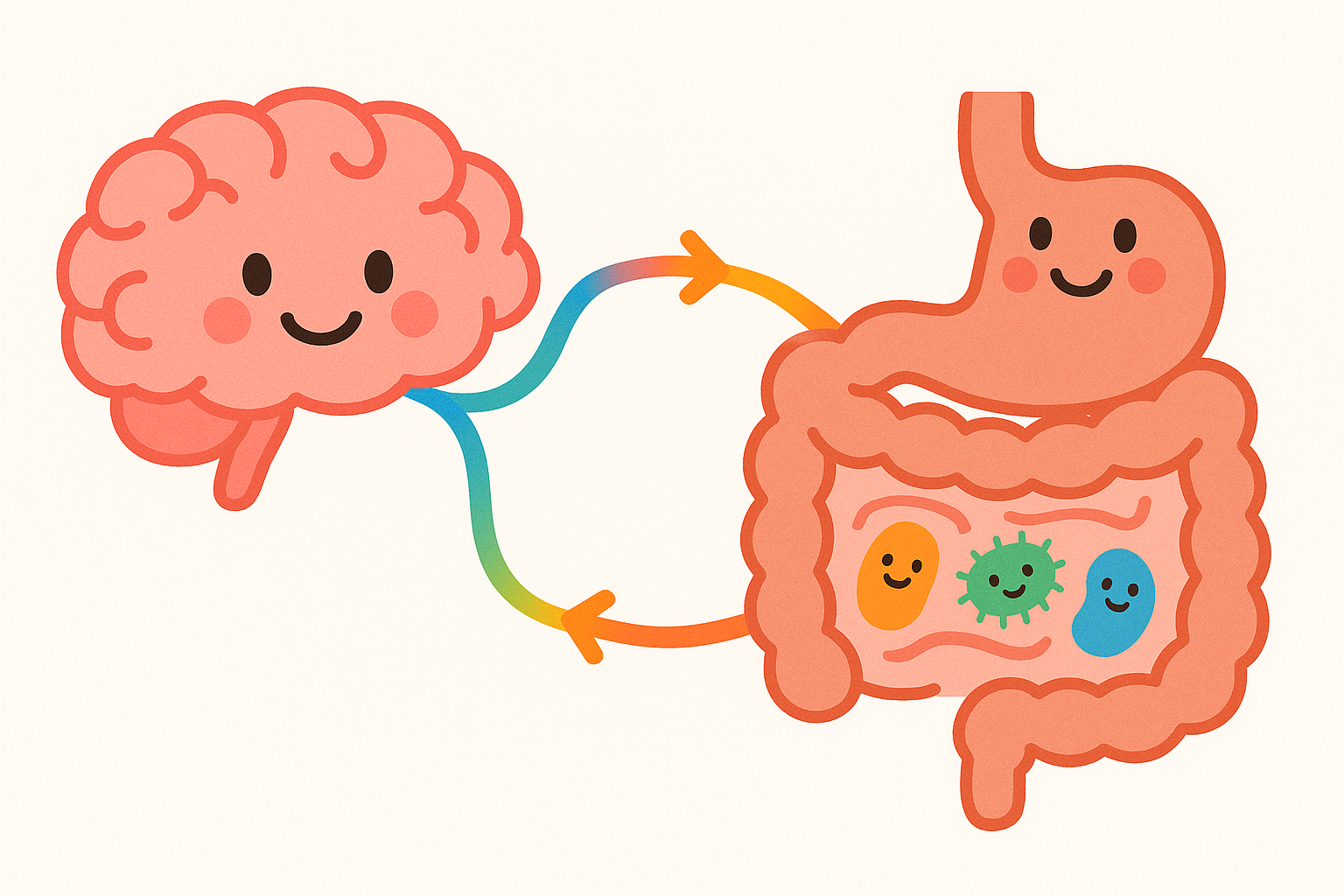
In recent years, researchers have focused on a specific area of this network called psychobiotics (sy-ko-by-AHT-iks). A psychobiotic is a live microorganism (like a probiotic) or a dietary fiber (like a prebiotic) that provides mental health benefits when consumed in adequate amounts.
The short answer to whether gut bacteria affect your mood is yes. Current science shows that the bacteria in your gut produce chemicals that communicate with your brain. By changing the balance of these bacteria, a growing body of research suggests we may be able to reduce symptoms of stress, anxiety, and depression.
How Do Gut Bacteria Talk to the Brain?
It might seem strange that microscopic organisms in your intestines can influence how you feel. However, research shows that gut bacteria use several distinct pathways to send messages to the brain.
The Vagus Nerve
The vagus nerve (VAY-gus nurv) is a long nerve that acts like a direct telephone line between your gut and your brain. It carries signals in both directions. Some gut bacteria can stimulate the nerve endings in the digestive tract, sending messages up to the brain that can influence anxiety and emotional behavior.
Neurotransmitter Production
Your brain relies on chemical messengers called neurotransmitters to regulate mood. Surprisingly, your gut bacteria produce many of these same chemicals. For example, gut bacteria produce large amounts of serotonin (sair-uh-TOE-nin), a chemical that regulates happiness and anxiety. They also produce GABA (GAB-uh), a chemical that helps calm the nervous system. While these gut-produced chemicals may not travel directly into the brain, they influence the local nervous system in the gut, which then signals the brain.
The Stress Response System
Your body handles stress using a system called the HPA axis (hypothalamic-pituitary-adrenal axis). When you are stressed, this system releases cortisol (KOR-tih-sol), the primary stress hormone. A 2025 review in Probiotics and Antimicrobial Proteins found that certain beneficial gut bacteria can actually turn down the activity of the HPA axis, resulting in lower cortisol levels and a calmer physical state.
Immune System and Inflammation
Your gut houses about 70 percent of your immune system. When the balance of good and bad bacteria in your gut is disrupted, it can lead to low-level inflammation. This inflammation can travel throughout the body and affect the brain. Scientists have strongly linked chronic inflammation to mental health conditions like depression. Related: Does Leaky Gut Syndrome Actually Exist? What the Latest Science Says
What the Research Shows
For a long time, most of the evidence supporting psychobiotics came from animal studies. Researchers found that mice raised in sterile environments without any gut bacteria showed exaggerated, abnormal reactions to stress. When these mice were given healthy gut bacteria, their stress responses returned to normal.

Today, scientists are conducting more human trials to see if these benefits apply to us.
Anxiety and Everyday Stress
Several studies show that psychobiotics can help people manage high-stress situations. A 2023 study in Frontiers in Immunology looked at 60 college students experiencing severe test anxiety. Half of the students took a specific probiotic strain called Lactobacillus plantarum JYLP-326, while the other half took a placebo. After three weeks, the students taking the probiotic showed significant reductions in anxiety, depression, and insomnia. The researchers also noted positive changes in their gut bacteria profiles.
Another study on medical students found that consuming milk fermented with Lactobacillus casei before a major exam led to lower cortisol levels and fewer physical stress symptoms compared to a placebo group.
Depression and Mood
People with depression often have different gut bacteria profiles compared to people without depression. A 2025 review in Current Nutrition Reports highlighted that depressed individuals frequently have lower levels of beneficial Bifidobacterium and Lactobacillus strains.
Clinical trials have tested whether replacing these bacteria can help. In multiple studies, healthy adults who took a daily multi-strain probiotic supplement reported less psychological distress, lower cortisol levels, and reduced negative thoughts compared to those taking a placebo.
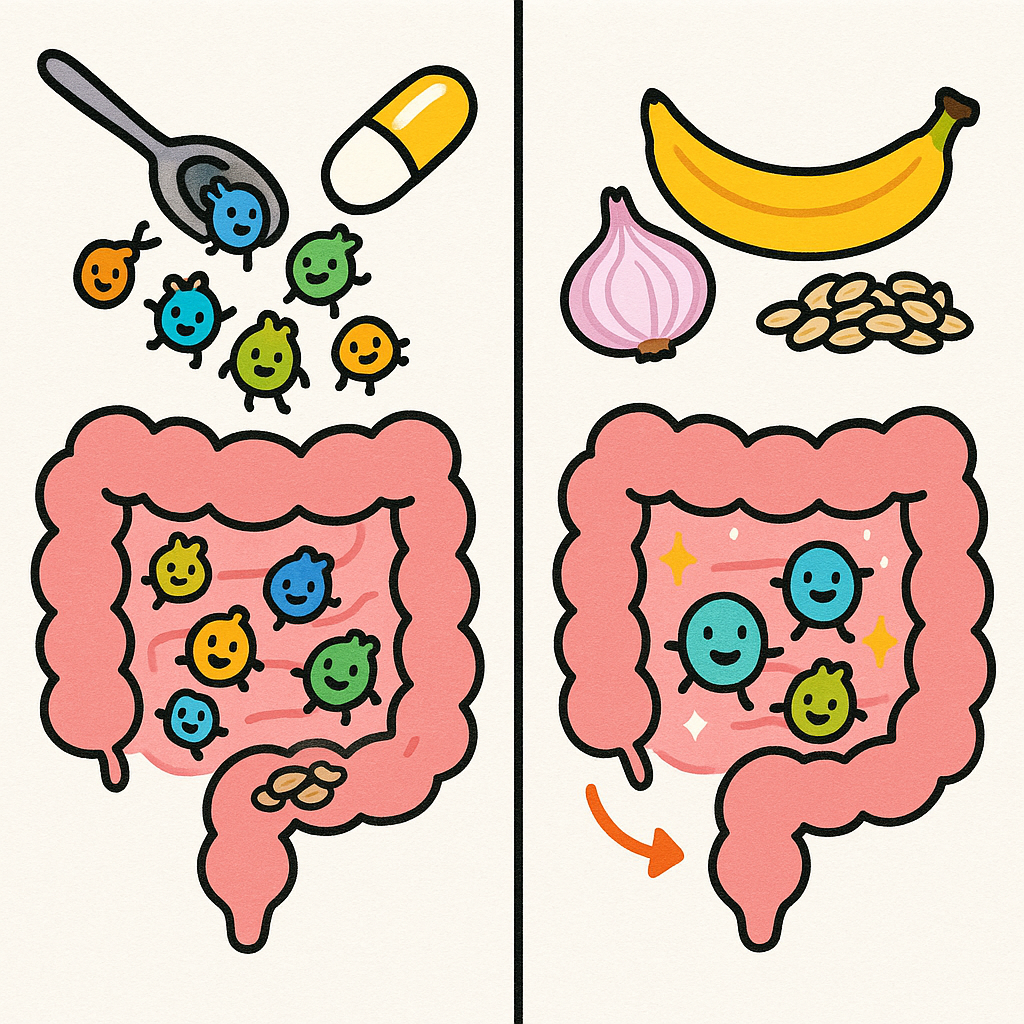
How Prebiotics Fit In
While probiotics are the actual live bacteria, prebiotics are the fibers that feed them. A 2016 review in Trends in Neurosciences noted that healthy volunteers who consumed specific prebiotics (like galacto-oligosaccharides) showed a reduced waking cortisol response. They also paid less attention to negative emotional stimuli, which is considered a sign of reduced anxiety.
| Feature | Probiotics | Prebiotics |
|---|---|---|
| What they are | Live, beneficial bacteria | Dietary fibers that humans cannot digest |
| Function | Add new beneficial microbes to the gut | Provide food to help existing good bacteria grow |
| Common Sources | Yogurt, kefir, kimchi, supplements | Garlic, onions, bananas, oats, specific supplements |
| Role in Mental Health | May produce mood-regulating chemicals | Help mood-regulating bacteria multiply and thrive |
Who Benefits Most and Who Needs Caution
The current science suggests that psychobiotics are most effective for individuals dealing with mild to moderate stress, everyday anxiety, and mild depressive symptoms.
However, psychobiotics are not a replacement for traditional psychiatric medications or therapy. They are generally viewed as a complementary approach.
Furthermore, research shows that psychobiotics may not be effective for severe, advanced neurological conditions. A 2021 clinical trial in Archives of Microbiology tested a probiotic combination on patients with severe Alzheimer’s disease. After 12 weeks, the researchers found no significant improvements in cognitive function or inflammation markers. This suggests that while gut bacteria influence the brain, altering them may not be enough to reverse advanced brain diseases.
Practical Guidance: Supporting Your Gut-Brain Axis
If you want to support your mental health through your gut, the research points to several actionable steps.
First, focus on your overall diet. The Mediterranean diet and the MIND diet are strongly associated with a healthy gut microbiome and a lower risk of depression. These diets are rich in fiber, whole grains, nuts, and vegetables, which act as prebiotics to feed your good bacteria.
Second, consider adding fermented foods to your routine. Foods like plain yogurt, kefir, sauerkraut, and kimchi naturally contain live bacterial strains that support gut health.
Finally, if you are considering a psychobiotic supplement, look for products containing specific strains that have been studied for mental health. Strains from the Lactobacillus and Bifidobacterium families are the most thoroughly researched for mood and anxiety benefits.
Common Questions About Psychobiotics
How long does it take for psychobiotics to work?
In most clinical trials, participants take psychobiotics daily for 3 to 8 weeks before researchers measure significant changes in mood or stress levels. It is not a quick fix and requires consistent daily use.
Can I just eat yogurt instead of taking a pill?
Yes, eating fermented foods like yogurt can provide beneficial bacteria. However, clinical trials often use highly concentrated, specific strains of bacteria in pill form to achieve targeted mental health results. Both approaches support gut health, but supplements offer more precise dosing.
Do antibiotics affect my mental health?
Antibiotics kill both bad and good bacteria in your gut. Some studies suggest that frequent antibiotic use can temporarily disrupt the gut-brain axis, which may influence mood. Related: What Science Actually Says About Fecal Transplants for Gut Health
The Bottom Line
The science of psychobiotics is a rapidly growing field that proves our mental health is deeply connected to our physical health. Evidence clearly shows that the bacteria in our gut communicate with our brain, influence our stress hormones, and impact our mood.
While psychobiotics are not a magic cure for severe psychiatric or neurological illnesses, they offer a promising, low-risk tool for managing everyday stress, anxiety, and mild depression. Eating a fiber-rich diet, consuming fermented foods, and potentially using targeted probiotic supplements can be an excellent way to support both your digestive and mental well-being.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Test Anxiety in Students | L. plantarum JYLP-326 reduced anxiety, depression, and insomnia in college students facing exams. | PMID 37033942 |
| Severe Alzheimer’s Disease | A 12-week probiotic trial showed no cognitive or biochemical improvements in patients with severe Alzheimer’s. | PMID 34923592 |
| Diet and Depression | Diets rich in fiber and prebiotics (like the Mediterranean diet) alter the microbiome and reduce the risk of depression. | PMID 39928205 |
| Prebiotics and Stress | Healthy adults taking prebiotics showed reduced waking cortisol and less attention to negative emotional stimuli. | PMID 27793434 |
| General Mental Health Review | Psychobiotics regulate the HPA axis, reduce inflammation, and produce neurotransmitters like GABA and serotonin. | PMID 40402417 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply