Predicting heart disease often feels like guesswork. For decades, doctors have relied on traditional risk factors like age, cholesterol levels, and blood pressure to estimate a person’s chances of having a heart attack. This is a bit like guessing the condition of the pipes inside your house by measuring the water pressure. It gives you a good idea, but it does not let you actually see inside the pipes.

A Coronary Artery Calcium (CAC) scan changes that. It is a quick, non-invasive CT scan that takes a direct look at the arteries supplying your heart to see if calcified plaque has built up.
So, what does the score actually mean? In short, a score of zero indicates a very low short-term risk of a heart attack, while higher scores indicate advanced plaque buildup that requires medical attention. However, researchers are learning that the test is not necessary for everyone.
Here is a breakdown of what the latest science says about coronary calcium scores, who benefits most from the test, and what the numbers really mean for your health.
How This Might Work: Why Is There Calcium in the Heart?
To understand a calcium score, it helps to understand how heart disease develops.
Atherosclerosis (ath-er-o-skluh-RO-sis) is the process where fats, cholesterol, and other substances build up in and on the artery walls. This buildup is called plaque.
When plaque first forms, it is soft. Over time, the body tries to heal this inflamed area by depositing calcium over it, much like a scab forming over a cut. This hardens the plaque. A CAC scan acts as a highly sensitive camera that lights up when it sees this calcium.
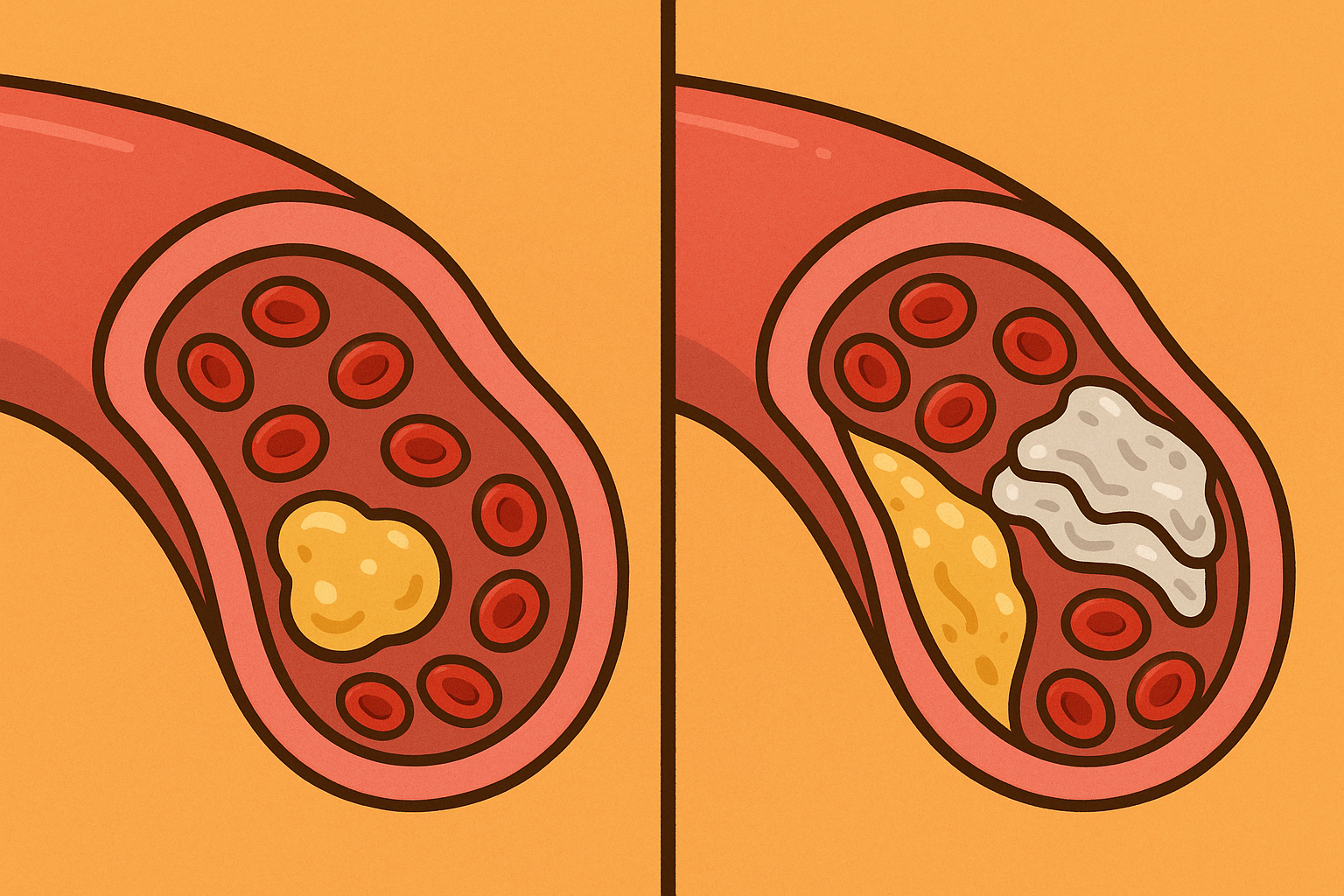
The results are calculated using the Agatston score (AG-at-ston), a standard point system developed in the 1990s that measures both the area and the density of the calcium in your coronary arteries.
What the Research Shows: Decoding the Score
When you get a CAC scan, you are given a number. Scientific research has consistently shown that as this number goes up, so does the risk of cardiovascular events.
The “Power of Zero”
If your score is zero, no calcified plaque was found. A 2016 review in Current Atherosclerosis Reports highlighted what cardiologists call the “warranty period.” For many asymptomatic people, a score of zero means the risk of dying from a heart-related event remains incredibly low (under 1%) for the next 10 to 15 years.
For some patients, a zero score can safely downgrade their perceived risk, potentially allowing them and their doctor to decide against starting daily cholesterol medications (statins).
Moderate to High Scores
As calcium accumulates, the risk rises. A 2004 meta-analysis in the Archives of Internal Medicine looked at over 13,000 patient-years of data and found that people with scores between 1 and 100 had double the risk of a heart event compared to those with a score of zero.
When scores get very high, the risk profile changes dramatically. A 2023 study in JACC: Cardiovascular Imaging examined over 4,500 people. They found that individuals with a CAC score over 300 had the exact same rate of major adverse cardiovascular events (like heart attacks) as people who had already survived a previous heart attack.
Quick Score Reference
| Agatston Score | Plaque Burden | General Clinical Interpretation |
|---|---|---|
| 0 | No calcified plaque | Very low risk. Statins may not be necessary for some. |
| 1 – 99 | Mild plaque | Low to moderate risk. Lifestyle changes recommended. |
| 100 – 299 | Moderate plaque | Moderate to high risk. Statins and aspirin often considered. |
| 300+ | Extensive plaque | High risk. Often treated as aggressively as existing heart disease. |
Who Benefits Or Needs Caution: The Timing of the Test
While the test is highly accurate at spotting calcium, it is not useful for everyone. A 2025 paper in JAMA Cardiology outlined a framework for doctors: the test is only helpful if it is not done “too early, too late, or too often.”
The Sweet Spot (Intermediate Risk)
The people who benefit the most are those at “intermediate risk.” If your doctor looks at your cholesterol, age, and blood pressure and is on the fence about whether you need a statin, the CAC score acts as the ultimate tie-breaker. A 2023 study in JAMA confirmed that adding a CAC score to traditional risk calculators significantly improves risk prediction in middle-aged and older adults.
Too Early
For young adults (under 40), the test is usually not recommended. Because it takes decades for soft plaque to calcify, a 35-year-old will almost always score a zero. However, they could still have dangerous soft plaque building up. In this group, a zero score might provide a false sense of security.
Too Late
If you have already had a heart attack, have a stent, or are already taking a high-dose statin, getting a CAC scan is generally considered “too late.” Your doctor already knows you have heart disease, and knowing your exact calcium score will not change your treatment plan.
Special Focus: People with Diabetes
People with Type 2 Diabetes are generally considered at high risk for cardiovascular disease. Because of this, doctors often prescribe statins automatically.
However, research shows a wide variation in actual risk. A 2022 study in Diabetes Care tracked over 6,700 participants. They found that patients with diabetes who had a CAC score of zero actually had a lifetime cardiovascular risk that overlapped with low-risk individuals without diabetes. Conversely, a 2020 study in The Journal of the Association of Physicians of India found that nearly 36% of completely asymptomatic diabetic patients had significant silent coronary artery disease revealed by a CAC scan. For diabetics, the scan can highly personalize treatment rather than relying on a one-size-fits-all approach. Related: Continuous Glucose Monitors: What the Latest Science Actually Says
Common Misunderstandings or Myths
Myth: A score of zero means you have no plaque.
A CAC scan only sees calcified plaque. It cannot see soft, newly formed plaque. While a zero score is an excellent sign, it does not guarantee your arteries are perfectly clear, especially if you are young or have a strong family history of early heart attacks.
Myth: Denser calcium is always worse.
It sounds logical that denser calcium would be more dangerous, but the opposite might be true. A 2016 review in JACC: Cardiovascular Imaging noted that denser plaques are often older, “healed,” and stabilized. Less dense, spread-out calcium might represent newer, active, and inflamed plaques that are more prone to rupturing and causing a clot.
Where The Science Is Still Uncertain
While CAC scoring is widely supported, there is some debate about its overall impact on population health.
A 2022 meta-analysis in JAMA Internal Medicine looked at whether adding CAC scores to standard risk calculators actually prevented heart attacks. The researchers found that while the score slightly improved mathematical risk prediction, most of the people who were reclassified into “high risk” categories did not actually go on to have a heart event during the 5 to 10-year follow-up. This suggests that while the test is good at finding plaque, we still need better ways to figure out exactly which plaques will cause heart attacks. Related: Can You Actually Reverse Arterial Plaque? What the Latest Science Says
Beyond the Basic Score
The Agatston score is over 25 years old, and scientists are finding new ways to extract data from the same CT scans.
- Fat-Omics: A 2024 study in Scientific Reports used artificial intelligence to analyze epicardial adipose tissue (ep-ih-KAR-dee-ul AD-ih-pohs TISH-oo): the fat stored directly around the heart. They found that measuring this fat, alongside the calcium, was highly effective at predicting heart failure, even outperforming standard clinical factors.
- Extra-coronary Calcification: Calcium doesn’t just build up in the coronary arteries. It can build up in the aortic valve or the thoracic aorta. Research shows that calcium in these other areas is also a strong predictor of overall mortality, acting as a sign of systemic, body-wide aging of the blood vessels.
The Bottom Line
The Coronary Artery Calcium score is one of the most powerful tools currently available to predict heart disease risk. By directly visualizing the arteries, it removes much of the guesswork from preventive cardiology.
- If you are at intermediate risk, a CAC scan can act as a tie-breaker to help you and your doctor decide if medications like statins are right for you.
- A score of zero provides a strong “warranty period” against near-term heart events, though it does not mean you are immune to soft plaque.
- A score over 300 suggests advanced disease that usually requires aggressive lifestyle and medical management.
- The test is not for everyone. If you are very young, already have known heart disease, or are already taking a statin, the test is unlikely to change your medical care.
Talk to a healthcare provider about whether your specific risk factors make you a good candidate for a coronary calcium scan.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Timing of CAC Testing | Outlined the “too early, too late, too often” framework for when CAC testing is actually clinically useful. | PMID 40042828 |
| High Scores & Risk | Found that asymptomatic patients with a CAC >300 have cardiovascular event rates equal to patients who already have established heart disease. | PMID 37227328 |
| CAC in Diabetes | Showed that diabetics with a CAC of 0 have a lifetime risk overlapping with low-risk non-diabetics, allowing for highly personalized care. | PMID 35168253 |
| AI and Fat-Omics | Used deep learning to show that analyzing heart fat alongside calcium predicts heart failure better than clinical factors alone. | PMID 39505933 |
| Reclassification Limits | A meta-analysis showing that while CAC improves risk prediction, many people reclassified as high-risk still do not experience heart events. | PMID 35467692 |
| Plaque Density | Highlighted that denser calcium might indicate healed, stable plaques, whereas lower density may pose a higher rupture risk. | PMID 27931526 |
Last updated: March 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.




Leave a Reply