Your skin is the ultimate boundary between you and the outside world. If your body is like a house, your skin is the roof, the insulation, and the security system all rolled into one. For decades, scientists viewed the outermost layer of the skin as a simple layer of dead cells. Today, research reveals a highly dynamic, living ecosystem where complex chemistry, microscopic water channels, and even invisible bacteria work together to keep moisture in and irritants out.
When this system works well, your skin feels smooth, hydrated, and calm. When it breaks down, the result is dryness, itching, and irritation. Understanding how the skin barrier functions can help you make better decisions about how to care for it.
What the Research Shows: The Brick and Mortar Structure
The primary physical barrier of your skin is the outermost layer of the epidermis, known as the stratum corneum (STRA-tum COR-nee-um, the horny outer layer of the skin). Scientists frequently use a “brick and mortar” analogy to describe how it works.

The “bricks” are flattened, tough cells called corneocytes. Inside these cells are proteins and natural sponge-like substances known as Natural Moisturizing Factor (NMF). NMF acts like a magnet for water, holding moisture inside the cells to keep them plump and elastic.
The “mortar” holding these cells together is a highly organized mixture of fats, or lipids. A 2016 review in Current Problems in Dermatology explains that this lipid matrix is made of three main components in roughly equal amounts: ceramides, cholesterol, and free fatty acids.
Ceramides are particularly important. A 2019 study in Biochimica et Biophysica Acta highlights the role of a specific enzyme called PNPLA1. This enzyme helps create a unique type of ceramide called an acylceramide. Acylceramides act as molecular rivets that physically link the layers of lipids together, creating a watertight seal. When genetic mutations impair this enzyme, it results in severe dry skin conditions, underscoring how vital these microscopic lipids are for retaining water.
How This Might Work: Hydration and The Acid Mantle
While the lipid mortar prevents water from escaping, the skin also has active mechanisms to pull water up from deeper layers.
Recent science has identified specialized water channels in the skin called aquaporins (ah-kwa-PORE-ins, proteins that form pores in cell membranes). A 2007 review in the Journal of Cosmetic Dermatology details how a specific channel, Aquaporin-3, transports both water and glycerol from the deeper, blood-rich layers of the skin up to the surface. Glycerol is a natural humectant, meaning it grabs onto water. Without these channels, the outer skin would quickly dry out, regardless of how much water you drink.
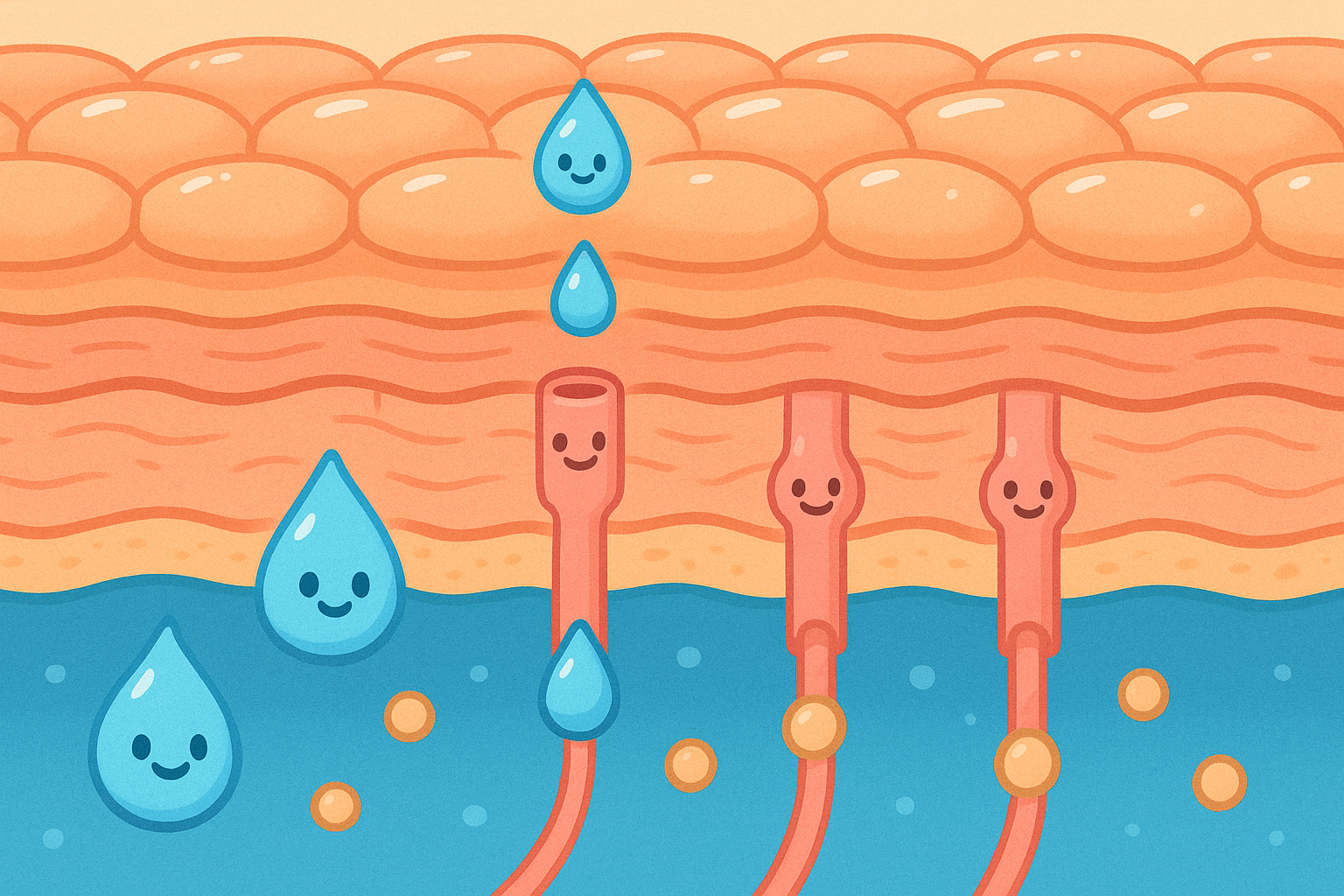
Another critical feature of a healthy barrier is its pH level. Healthy skin is slightly acidic. This “acid mantle” is necessary for the enzymes that produce ceramides to function properly. A 2014 systematic review in Archives of Dermatological Research tracked the skin barrier function in infants during their first two years of life. Researchers found that babies are born with a relatively neutral skin pH. However, during the very first week of life, their skin pH drops steeply, creating the acidic environment necessary to defend against harmful bacteria and build a mature, protective barrier.
The Surprising Role of Bacteria and Hair Follicles
We often think of skin bacteria as something to wash away, but research shows that certain microbes are active partners in building your skin barrier.
For example, Cutibacterium acnes is a bacterium usually associated with acne. However, a 2023 study in Science Advances revealed a surprising benefit to its presence on healthy skin. As this bacterium digests natural skin oils, it produces short-chain fatty acids, specifically propionic acid. This acid acts as a chemical signal that tells your skin cells to ramp up their production of essential barrier lipids, including triglycerides and ceramides. In this way, normal levels of skin bacteria actively help waterproof your skin.
Related: The Science of Your Skin Microbiome: How Invisible Bacteria Protect You
Additionally, the barrier is not just a flat sheet. It dips down into your hair follicles. A 2024 study in Cell Reports demonstrated that the upper hair follicle forms its own functional barrier. When researchers disrupted the barrier inside the hair follicle, the surrounding flat skin reacted by ramping up its own defense proteins. The follicle also serves as a critical passageway for sebum (natural skin oil) to reach the surface, adding another layer of protection to the outer barrier.
Who Benefits Or Needs Caution: Eczema and Aging
When the skin barrier fails, water evaporates into the air too quickly. Dermatologists measure this using a metric called transepidermal water loss (trans-ep-ih-DER-mal water loss, the amount of water that passively evaporates through the skin to the outside environment). High water loss is a hallmark of dry skin and conditions like atopic dermatitis (eczema).
In people with atopic dermatitis, the physical structure of the barrier changes. The 2016 review in Current Problems in Dermatology notes that in eczema-prone skin, the lipid chains are physically shorter. Instead of packing tightly together in a dense grid, they pack loosely. This loose arrangement allows water to slip through the cracks and evaporate.
Interestingly, the skin barrier also operates on a biological clock. A 2024 pilot study in the Journal of Biological Rhythms observed that in healthy individuals, the skin barrier naturally tightens and retains water better in the evening. However, in patients with atopic dermatitis, this rhythm is reversed. Their barrier function worsens at night, leading to a spike in water loss. This nighttime barrier failure is strongly linked to the severe evening itch that many eczema patients experience.
Age also plays a role in barrier health. A 2015 review in Cold Spring Harbor Perspectives in Medicine explains that as we undergo natural chronological aging and accumulate sun exposure, epidermal cell renewal slows down. The deeper collagen matrix fragments, and the skin loses its ability to hold onto moisture as effectively as it once did.
Related: Anti-Aging Skincare and Procedures: What Science Actually Shows
Practical Guidance: How Science Approaches Skin Repair
When the barrier is compromised, topical treatments can help restore function. A 2003 review in the American Journal of Clinical Dermatology outlines how different ingredients in moisturizers physically alter the skin barrier to reduce water loss.
Moisturizers generally rely on three types of ingredients to repair the barrier:

1. Humectants: Ingredients like urea, lactic acid, and glycerin act like molecular sponges. They penetrate the outer layers of the stratum corneum and attract water from the deeper layers of the skin, holding it in place.
2. Occlusives: Ingredients like petrolatum (petroleum jelly) sit on top of the skin and create a physical, waterproof seal. This prevents water from evaporating into the air, giving the underlying skin cells time to repair their own lipid mortar.
3. Emollients: These are oils and fats that sink into the microscopic cracks between the dry, curling corneocyte bricks. They smooth the surface, making the skin feel soft and flexible.
Research shows that using a combination of these ingredients is most effective. Applying pure lipids (like plain ceramides) without the right ratio of cholesterol and fatty acids can sometimes disrupt the barrier further. However, properly formulated moisturizers integrate directly into the skin’s natural lipid matrix, accelerating repair.
Beyond basic moisture, vitamins also play a supportive role. A 2017 review in Nutrients highlights that Vitamin C is actively transported into the epidermis, where it promotes the formation of collagen and scavenges free radicals generated by UV exposure and pollution, protecting the barrier from oxidative damage.
Related: Protecting Skin From UV Damage: What the Latest Science Says
Common Questions About the Skin Barrier
Does drinking more water hydrate dry skin?
While severe dehydration affects the whole body, drinking excess water does not cure dry skin. Skin hydration is primarily determined by how well your outer skin barrier can trap and hold water, not just how much water is circulating inside your body.
Why does my skin feel dry after a hot shower?
Hot water and harsh soaps can melt and wash away the natural lipid “mortar” and Natural Moisturizing Factors that hold your barrier together. Washing with lukewarm water and applying a moisturizer immediately afterward helps lock the absorbed water into the skin before it can evaporate.
The Bottom Line
The skin barrier is far more than a passive shield. It is an intricate, living wall made of tightly packed cells, complex fats, water channels, and beneficial bacteria.
- What we know: The barrier depends on a precise mixture of ceramides, cholesterol, and fatty acids to prevent water loss. An acidic pH and a healthy microbiome actively support the production of these protective fats.
- What remains uncertain: Scientists are still mapping exactly how internal circadian clocks regulate skin hydration, and why this rhythm breaks down in conditions like eczema.
- How to protect it: You can support your skin barrier by avoiding harsh, lipid-stripping cleansers and using moisturizers that combine humectants (to draw water in) and occlusives (to trap water inside).
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Skin Bacteria | C. acnes produces short-chain fatty acids that trigger skin cells to produce more barrier-protecting lipids. | PMID 37595033 |
| Circadian Rhythms | Healthy skin retains water better at night, but skin with atopic dermatitis loses more water in the evening, leading to nocturnal itching. | PMID 38305093 |
| Infant Skin Development | Babies are born with a neutral skin pH that drops steeply in the first week to form a protective acid mantle. | PMID 24595645 |
| Eczema and Lipids | In atopic dermatitis, skin lipids are physically shorter and packed loosely, allowing water to easily escape. | PMID 26844894 |
| Skin Hydration | Aquaporin-3 proteins act as microscopic channels to pull water and glycerol from deep tissues into the outer skin layers. | PMID 17524122 |
| Hair Follicles | The upper hair follicle forms its own functional barrier and helps regulate the surrounding skin’s defense systems. | PMID 38941190 |
Last updated: May 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.


Leave a Reply