In the 1670s, a Dutch scientist named Antonie van Leeuwenhoek scraped a small amount of plaque from his teeth, placed it under a microscope of his own design, and discovered tiny living creatures darting around. He had just caught the first glimpse of the oral microbiome.
Today, scientists know that the human mouth is home to the second largest microbial community in the body, trailing only the gut. Your mouth hosts over 700 different species of bacteria, along with fungi, viruses, and other microscopic life forms.
For decades, dental care focused primarily on destroying these microbes to prevent cavities and gum disease. However, modern research reveals a much more complex picture. We now know that a healthy mouth relies on a delicate balance of microbes. When this balance is disrupted, it does not just affect your teeth and gums. The bacteria in your mouth can travel throughout your body, influencing your respiratory health, your digestive system, and even your brain.
This article synthesizes the latest scientific research to explain how the oral microbiome works, how it affects your systemic health, and what science actually says about keeping it balanced.
The Architecture of Your Mouth’s Ecosystem
To understand how the oral microbiome affects your health, it helps to understand how it is structured. The mouth is not a single, uniform environment. It is a diverse landscape with many different neighborhoods.
Bacteria that thrive on the hard, non-shedding surface of your teeth are entirely different from the bacteria that prefer the soft, oxygen-rich tissue of your cheeks or the deep, low-oxygen crevices of your gums.
A 2024 review in Nature reviews. Microbiology highlights that these microbes do not just float around randomly. They build highly organized, microscopic cities called biofilms. Using advanced imaging, researchers have seen bacteria arrange themselves into specific shapes, such as “corncob” structures where different species of bacteria physically attach to one another. This physical closeness allows them to share nutrients and protect each other from threats.
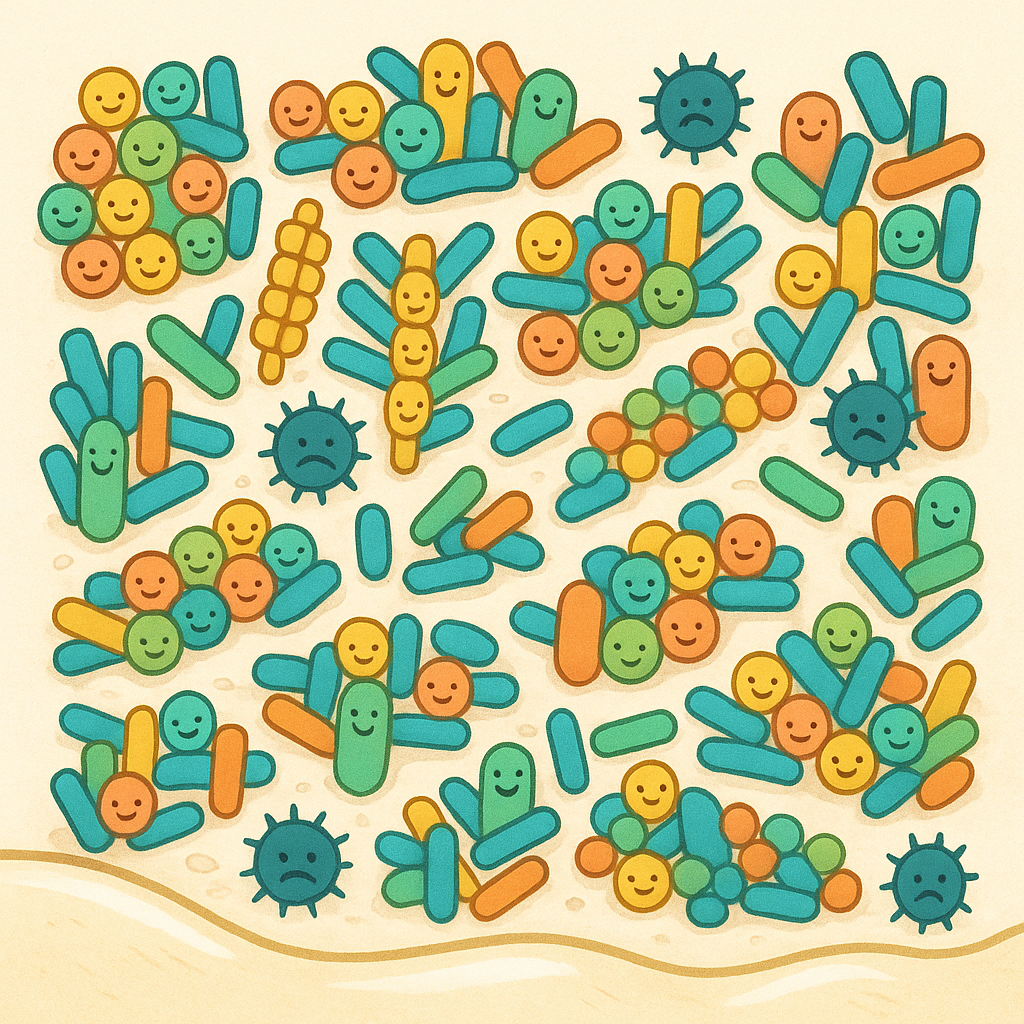
When this microscopic city is peaceful and balanced, it helps protect your mouth. Beneficial bacteria can crowd out harmful invaders, regulate the pH (acid level) of your saliva, and even help process nutrients.
However, poor diet, poor oral hygiene, or certain medications can cause this ecosystem to collapse. This leads to dysbiosis (dis-by-OH-sis), which is a state of microbial imbalance where harmful bacteria multiply and overpower the helpful ones.
What the Research Shows: The Systemic Impact
When dysbiosis occurs, the consequences extend far beyond bad breath or a cavity. Harmful bacteria, and the inflammation they trigger, can spread from the mouth to other parts of the body.
The Oral-Gut-Brain Axis
You swallow roughly one liter of saliva every day. Along with that saliva, you swallow thousands of oral bacteria. While stomach acid kills many of these microbes, some survive and travel into your intestines.
A 2024 study in Nutrients explored the “oral-gut-brain axis.” The researchers noted that in healthy individuals, the gut and the mouth have distinct microbial communities. However, in states of disease, oral bacteria frequently colonize the gut. For example, oral bacteria have been found in the guts of people with Inflammatory Bowel Disease (IBD) and colorectal cancer.
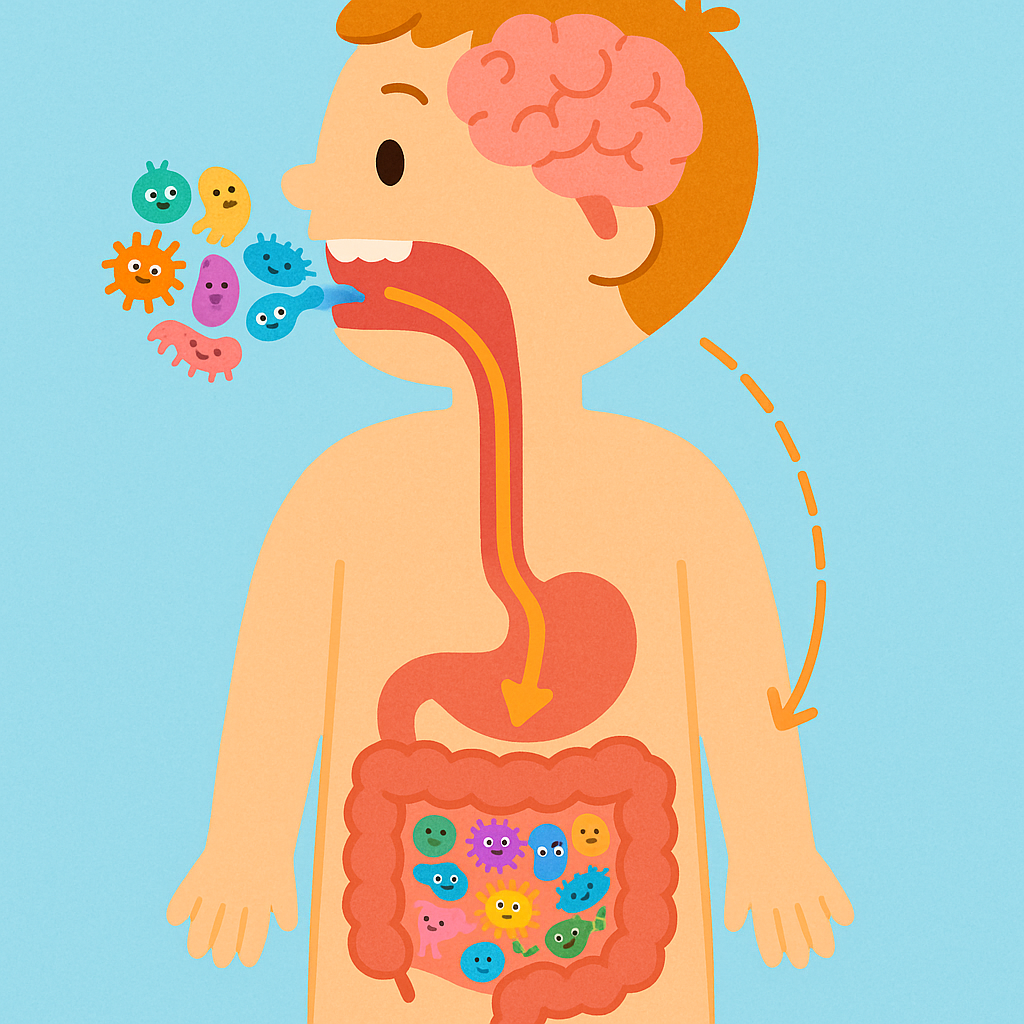
Furthermore, this connection extends to the brain. Harmful oral bacteria, particularly those that cause severe gum disease, have been detected in the brains of patients with Alzheimer’s disease. While scientists are still investigating exactly how these bacteria influence cognitive decline, the current theory suggests that chronic inflammation starting in the mouth can contribute to inflammation in the brain.
Related Reading: How the Gut-Brain Connection Actually Works: What the Latest Science Says
Respiratory Health and Pneumonia
Because the mouth is the gateway to the respiratory tract, oral bacteria have a direct path to the lungs. A 2021 review in Respiratory medicine details how microscopic droplets of saliva are constantly inhaled into the airways.
In healthy individuals, the immune system clears these microbes away. But in older adults, individuals with compromised immune systems, or those with chronic lung conditions, these inhaled oral bacteria can cause serious infections.
This is particularly relevant for aspiration pneumonia. A 2023 review in Clinics in geriatric medicine emphasizes that poor oral hygiene is a major risk factor for aspiration pneumonia in elderly populations. When dental plaque builds up, it acts as a reservoir for respiratory pathogens. Simply improving daily oral hygiene in nursing home residents has been shown to significantly reduce the rates of fatal pneumonia.
Pregnancy and the Oral Microbiome
During pregnancy, a woman’s body undergoes massive hormonal shifts. These hormones, particularly estrogen and progesterone, actually change the environment of the mouth and alter the microbiome.
A 2021 review in Journal of reproductive immunology explains that the total number of oral microbes increases during pregnancy. Additionally, the hormonal changes make the gums more sensitive to plaque, leading to a common condition known as “pregnancy gingivitis.”
If this progresses to periodontitis (pear-ee-oh-don-TIE-tis), a severe gum infection, it can pose risks to the pregnancy. Research shows that inflammation and bacteria from infected gums can enter the mother’s bloodstream and travel to the placenta. This systemic inflammation has been linked to a higher risk of preterm birth and low birth weight.
Common Misunderstandings About Mouthwash
Given the risks of harmful oral bacteria, it seems logical to use strong antibacterial mouthwashes to eliminate them. However, recent science suggests this “scorched earth” approach may do more harm than good.
A 2023 review in International dental journal looked closely at how over-the-counter mouthwashes affect the oral microbiome. Products containing chlorhexidine or high levels of alcohol kill bacteria indiscriminately. They wipe out the harmful bacteria that cause plaque, but they also destroy the beneficial bacteria that maintain oral health.
One of the most surprising discoveries is the role oral bacteria play in cardiovascular health. Certain beneficial bacteria on your tongue convert nitrates from your diet (found in leafy greens and beets) into nitrites. When you swallow these nitrites, your body converts them into nitric oxide, a molecule that helps relax blood vessels and lower blood pressure.
Studies show that using strong antibacterial mouthwash twice a day can wipe out these helpful bacteria, leading to a measurable increase in blood pressure. Therefore, researchers suggest that the ideal oral care routine should focus on “balancing” the microbiome rather than simply sterilizing the mouth.

How Dental Treatments Affect Your Microbiome
Everything you put in your mouth has the potential to alter your microbial ecosystem, including dental treatments.
Clear Aligners and Braces
The demand for clear orthodontic aligners has skyrocketed because they are nearly invisible. However, they drastically change the physical environment of the teeth.
A 2023 review in International dental journal found that while clear aligners generally result in better gum health than traditional metal braces (because they can be removed for brushing), they present their own challenges. Aligners create a closed, oxygen-deprived environment over the teeth and block saliva from naturally washing away food particles and neutralizing acids.
Researchers found that the inner surface of the plastic aligner trays can harbor specific types of bacteria, including Streptococcus, which are associated with cavities. To prevent this, the research suggests that patients must use both mechanical cleaning (brushing the trays) and chemical cleaning to disrupt the biofilms that stick to the plastic.
Related Reading: What Science Actually Says About the Health Benefits of Probiotics
Practical Guidance: Supporting a Healthy Oral Microbiome
The goal of modern oral care is to cultivate a diverse, balanced ecosystem where beneficial microbes keep harmful pathogens in check. Based on the synthesized research, here is how to support that balance:
Diet matters for your mouth, not just your gut: A diet high in refined carbohydrates and sugars feeds acid-producing bacteria like Streptococcus mutans*. These bacteria produce acids that erode tooth enamel. Conversely, a diet rich in fiber and whole foods promotes a more diverse and resilient microbial community.
- Be mindful of mouthwash: Unless prescribed by a dentist for a specific short-term infection, avoid using harsh, alcohol-based or chlorhexidine mouthwashes daily. They can disrupt your microbiome and potentially impact your blood pressure.
Consider oral probiotics: A 2023 review in Frontiers in cellular and infection microbiology notes that certain probiotic strains, specifically Lactobacillus and Bifidobacteria*, show promise in oral health. When taken as lozenges or in fermented foods, these beneficial bacteria can compete with cavity-causing pathogens for space and nutrients on the teeth.
- Maintain mechanical cleaning: The most effective way to manage biofilms without destroying the entire ecosystem is mechanical disruption. Regular brushing and flossing break up the structure of the plaque biofilm, preventing it from maturing into a state of dysbiosis.
Where The Science Is Still Uncertain
While we know that oral bacteria are present in systemic diseases, scientists are still working to understand the exact mechanisms of cause and effect.
For example, researchers have found the oral bacteria Porphyromonas gingivalis in the brains of Alzheimer’s patients and the tumors of colorectal cancer patients. However, it is still debated whether the bacteria actually caused the disease, or if the disease created a weakened environment that allowed the bacteria to easily settle there.
Additionally, the study of the oral “virome” (the viruses that live in the mouth) and the “mycobiome” (the fungi in the mouth) is still in its infancy. Most current research focuses heavily on bacteria, but future studies will likely reveal that fungi and viruses play equally important roles in maintaining oral balance.
The Bottom Line
Your mouth is not just a set of teeth and gums, it is a complex, living ecosystem that acts as the primary gateway to your body.
The research clearly shows that maintaining a balanced oral microbiome is critical for overall health. When the microbial community in your mouth falls into a state of dysbiosis, it can increase your risk for respiratory infections, pregnancy complications, and inflammatory conditions in the gut and brain.
Rather than trying to sterilize the mouth with harsh chemicals, the best approach is to support the beneficial bacteria through a healthy diet, consistent mechanical cleaning (brushing and flossing), and regular dental checkups.
Quick Reference: Key Studies
| Study Focus | Key Finding | Source |
|---|---|---|
| Oral Microbiome Overview | The mouth contains highly structured biofilms and dysbiosis is linked to systemic diseases. | PMID 37700024 |
| Oral-Gut-Brain Axis | Oral microbes can translocate to the gut and brain, influencing systemic biological aging and mental health. | PMID 39339804 |
| Clear Aligners | Aligners trap specific bacteria on their inner surfaces, requiring specific mechanical and chemical cleaning to prevent cavities. | PMID 37105789 |
| Oral Probiotics | Lactobacillus and Bifidobacteria can help reduce cavity-causing bacteria and prevent yeast infections in the mouth. | PMID 36968114 |
| Mouthwash Effects | Harsh mouthwashes can kill beneficial nitrate-reducing bacteria, potentially impacting cardiovascular health. | PMID 37867065 |
| Respiratory Health | Poor oral hygiene allows oral bacteria to be aspirated into the lungs, increasing the risk of pneumonia and COPD exacerbations. | PMID 34049183 |
| Pregnancy Complications | Hormonal shifts change the oral microbiome, and severe gum disease is linked to preterm birth and low birth weight. | PMID 33676065 |
| Aspiration Pneumonia | Improving daily oral hygiene in elderly populations significantly reduces the risk of fatal pneumonia. | PMID 37045532 |
Last updated: April 2026
This article synthesizes findings from peer-reviewed research. It is for educational purposes only and does not constitute medical advice. Consult a healthcare provider before starting any new regimen.



Leave a Reply